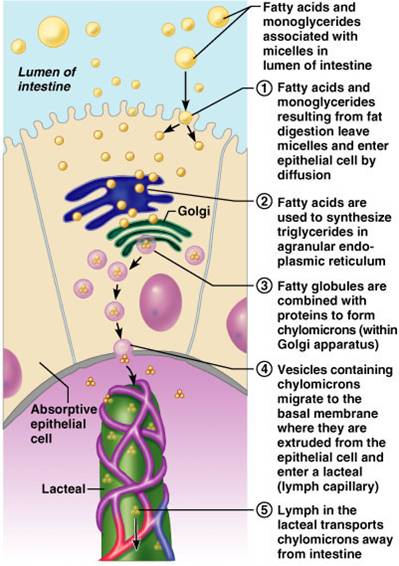
Regulation of Digestion
The GI tract is regulated by
1. An intrinsic set of nerves known as the enteric nervous system
2. By an extrinsic set of nerves that are part of the autonomic nervous system
Enteric Nervous System (ENS)
- Made of about 100 million neurons that extend from the esophagus to the anus
- The neurons are arranged into 2 plexuses, both made of motor neurons, interneurons, and sensory neurons:
1. Myenteric Plexus (also called plexus of Auerbach)
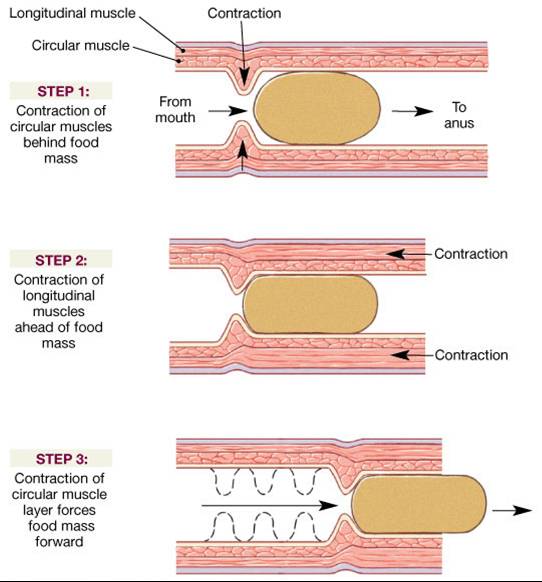
- Is located between the longitutidnal and circular smooth muscle layers of the muscularis
- The motor neurons mostly control GI tract motility (movement), particularly the frenquency and strength of contraction of the muscularis.
2. Submucosal Plexus (also called plexus of Meissner) is found within the submucosa
- The motor neurons supply the secretory cells of the mucosal epithelium, controlling the secretions of the organs of the GI tract
- Interneurons interconnect the neurons of the myenteric and submucosal plexuses
- Sensory neurons are chemoreceptors (receptors activated by the presence of certain chemicals in food located in the lumen of a GI organ) or stretch receptors (receptors activated when food distends-stretches- the wall of a GI organ)
- The neurons of the NS can function independently, but are subject to regulation by the neurons of the autonomic nervous system.
Autonomic Nervous System
- Vagus nerves (CN X) supply parasympathetic fibers to most parts of the GI tract (except last half of large intestine which has parasympathetic fibers fromm the sacral spinal cord)
- The nerves form neural connections with the ENS
- In general, stimulation of the parasympathetic nerves cause an increase in GI secretion and motility by increasing the activity of the ENS neurons while stimulation of sympathetic nerves has opposite effect
- Emotions such as anger, fear, and anxiety may slow digestion because they stimulate the sympathetic nerves that supply the GI tract
Segmentation and peristalsis are largely automatic involving local short reflex arcs linked to the CNS extrinsic controls via long autonomic reflex arc
Intrinsic Controls
- Regulated by local centers
- Autonomous (exist independently) smooth muscle pacesetter cells
- Intrinsic nerve plexuses and sensory receptors
- The visceral smooth muscle networks of the GI tract show rhythmic cycles of activity in the absence of neural stimulation. Pacesetter cells undergo spontaneous depolarization and trigger the contraction of entire muscular sheets.
- Autonomous Smooth Muscle
- Pacesetter cells generate slow wave potentials, the GI’s basic electrical rhythm (BER), wavelike fluctuations in membrane potential, transmitted throughout smooth muscle via gap junctions
- Threshold is reached by the effect of various mechanical, neural and hormonal factors in GI tract
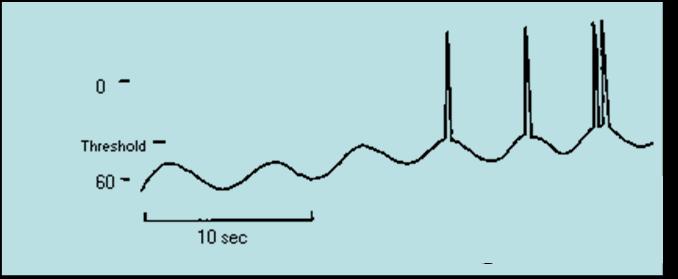
- Mechano- and chemoreceptors respond to:
- Stretch, osmolarity, and pH
- Presence of substrate, and end products of digestion
They initiate reflexes that:
- Activate or inhibit digestive glands
- Mix lumen contents and move them along
Neuronal Control
- Intrinsic controls
- Nerve plexuses near the GI tract initiate short reflexes
- Short reflexes are mediated by the enteric nervous system
- Extrinsic controls
- Long reflexes arising within or outside the GI tract
- Involve CNS centers and extrinsic autonomic nerves
- Parasympathetic reflexes
Extrinsic Controls
- Neural and hormonal mechanisms coordinate glands
- Autonomic nervous system (ANS) parasympathetic reflexes
- GI hormones enhance or inhibit smooth muscle contraction
Control of Digestion is Regulated By:
- Neural and hormonal mechanisms coordinate glands
- Hormonal mechanisms enhance or inhibit smooth muscle contraction
- Local mechanisms coordinate response to changes in pH or chemical stimuli
Oral Cavity Functions
- Analysis of material before swallowing by touch, temperature, and taste receptors
- Mechanical processing by the teeth, tongue, and palatal surfaces
- Lubricating food by mixing it with mucus and saliva
- Begins the digestion of carbohydrates with salivary enzymes
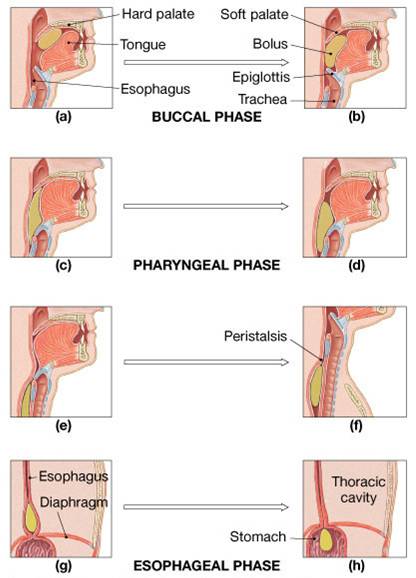
- Assists in swallowing
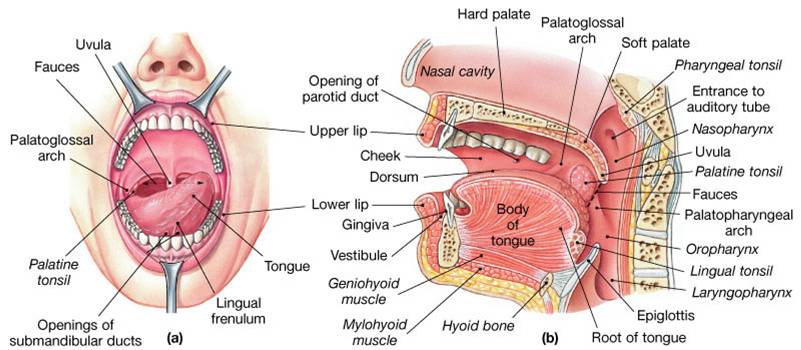
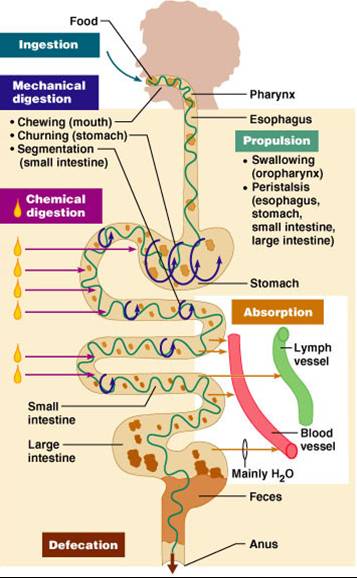
Digestive Processes in the Mouth
- Food is ingested
- Mechanical digestion begins (chewing)
- Propulsion is initiated by swallowing
- Salivary amylase begins chemical breakdown of starch
- The pharynx and esophagus serve as conduits to pass food from the mouth to the stomach
- Uvula guards opening to pharynx
Saliva
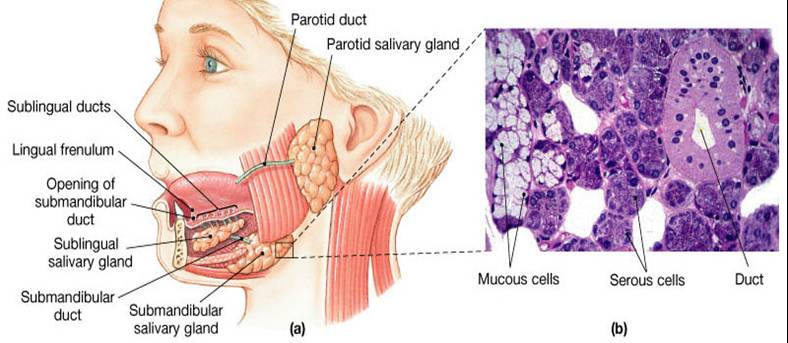
- 3 pairs of salivary glands (3 pairs) - parotid, sublingual, and submandibular
- Produce saliva - watery solution includes electrolytes, buffers, glycoproteins, antibodies, enzymes
- Functions include:
- Lubrication,
- Dissolving
- Initiation of digestion of complex carbohydrates (starches)
Saliva: Source and Composition
- Secreted from serous and mucous cells of salivary glands
- Made of 97-99.5% water
- Is a hypo-osmotic, slightly acidic solution containing
- Electrolytes – Na+, K+ Cl–, PO42, HCO3–
- Digestive enzyme – salivary amylase
- Proteins – mucin, lysozyme, defensins, and IgA
- Metabolic wastes – urea and uric acid
Control of Salivation
- Intrinsic glands keep the mouth moist
- Extrinsic salivary glands secrete serous, enzyme-rich saliva in response to:
- Ingested food which stimulates chemoreceptors and pressoreceptors
- The thought of food
- Strong sympathetic stimulation inhibits salivation and results in dry mouth
|
Functions of the Stomach
- Holds ingested food (at this point called chyme)
- Passes chyme in small increments to the small intestine
- Degrades food physically
- Begins digestion of proteins using enzyme called pepsin
- Secretes intrinsic factor required for absorption of vitamin B12
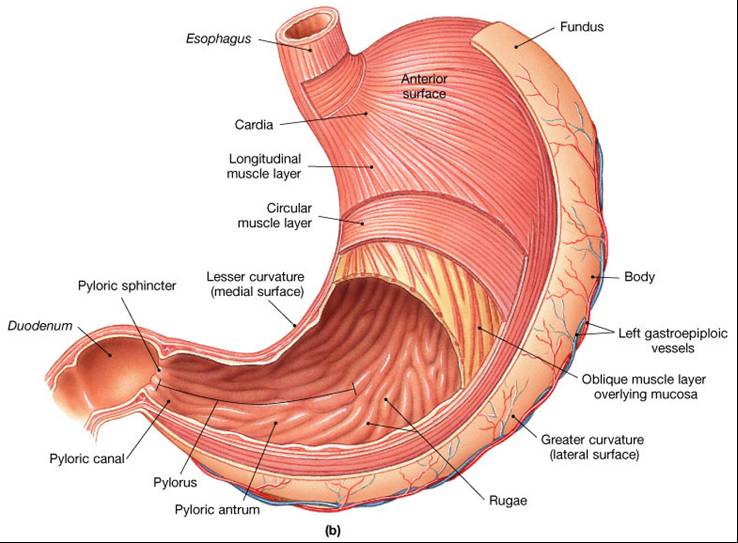
Stomach Lining
The stomach is exposed to the harshest conditions in the digestive tract
To keep from digesting itself, the stomach has a mucosal barrier with:
- A thick coat of bicarbonate-rich mucus on the stomach wall
- Epithelial cells that are joined by tight junctions
- Gastric glands that have cells impermeable to HCl
- Damaged epithelial cells are quickly replaced
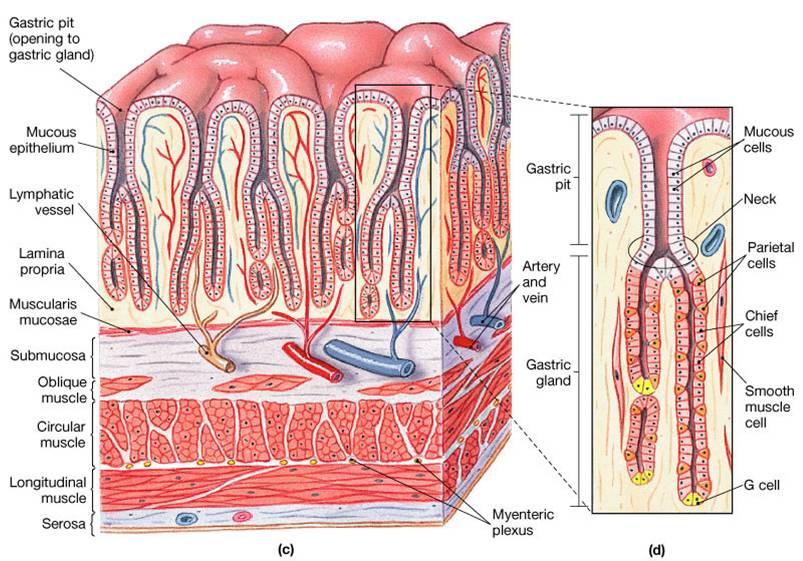
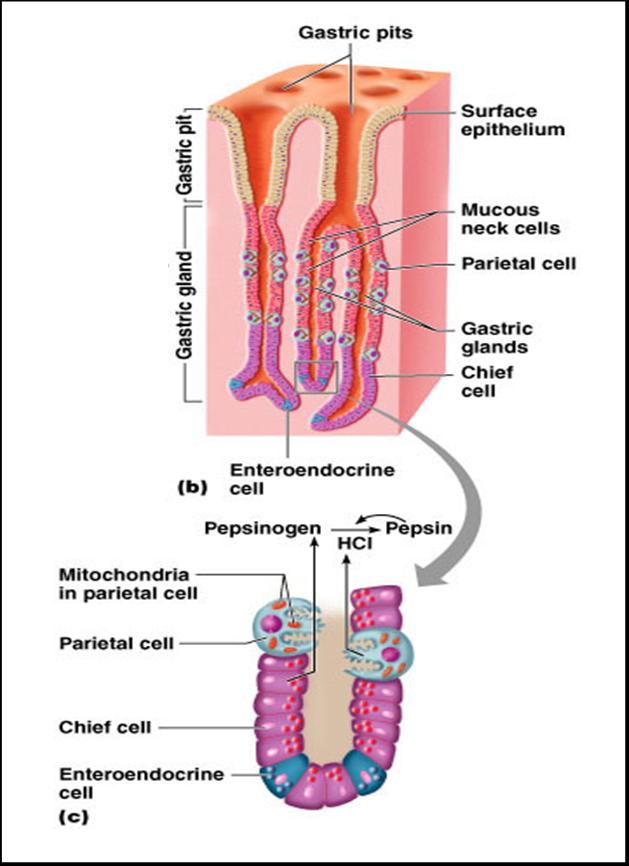
Gastric Glands of the Stomach
Gastric glands have a variety of secretory cells:
- Mucous Neck Cells
- secrete an alkaline mucus to protect the stomach lining from acidic gastric juice
- Chief Cells
- secrete the inactive enzyme called pepsinogen; pepsinogen is activated to pepsin by:
- HCl in the stomach
- Pepsin itself via a positive feedback mechanism
- Parietal Cells
- secrete hydrochloric acid (HCl) which helps convert pepsinogen into pepsin and kills microbes in food
- secretes intrinsic factor which helps with absorption of vitamin B12
- G Cells (Enteroendocrine Cells)
- secrete
several hormones and substances
- gastrin
- histamine
- endorphins
- serotonin
- cholecystokinin (CCK)
- somatostatin
Regulation of Gastric Secretion
- Neural and hormonal mechanisms regulate the release of gastric juice
- Stimulatory and inhibitory events occur in 3 phases:
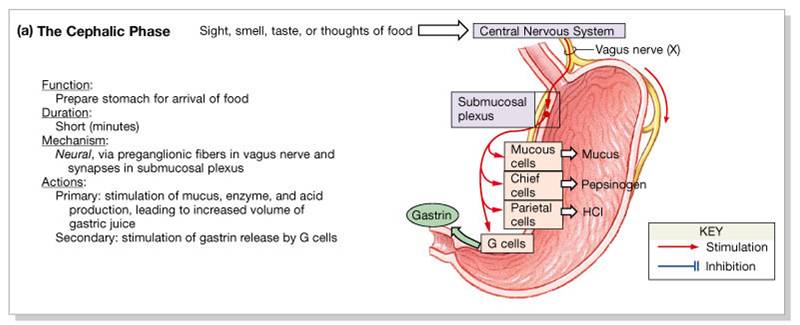
1. Cephalic (Reflex) Phase:
- Begins prior to food entry
- Prepares stomach to receive ingested material
- Increases production of gastric juices (saliva, gastric secretions, and pancreatic secretions)
- Excitatory events include
- Sight or thought of food
- Stimulation of taste or smell receptors
- Inhibitory events include
- Loss of appetite or depression
- Decrease in stimulation of parasympathetic division
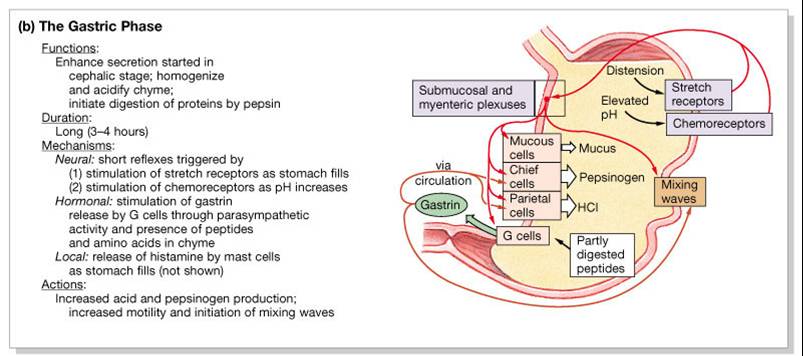
2. Gastric Phase:
- Begins with the arrival of food in the stomach
- Once food enters the stomach
- Neural, hormonal – secretion of gastrin
- pH drops (stimulated parietal cells) which triggers chemoreceptors to send a nerve impulse along the vagus nerve to the medulla oblongata
- Stomach wall stretches which triggers stretch receptors to sed a nerve impulse along the vagus nerve to the medulla oblongata
- Excitatory events include:
- Stomach distension - activation of stretch receptors (neural activation)
- Activation of chemoreceptors by peptides, caffeine, and rising pH
- Release of gastrin to the blood
- Inhibitory events include:
- a pH lower than 2
- Emotional upset that overrides the parasympathetic division
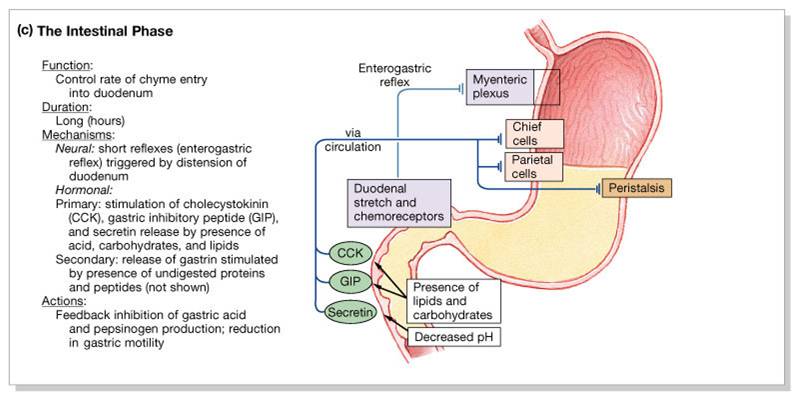
3. Intestinal Phase:
- Begins as partially digested food enters the duodenum
- Stretch receptors and chemoreceptors in the duodenum stimulate relfex pathways through the medulla that initially lead to more gastric secretion, gastric motility, and emptying of the stomach
- Release of hormones controls (inhibits) the rate of gastric emptying by releasing
- Excitatory phase
- low pH; partially digested food enters the duodenum and encourages gastric gland activity
- Inhibitory phase
- distension of duodenum and/or the presence of fatty, acidic, or hypertonic chyme, and/or irritants in the duodenum initiates inhibition of local reflexes and vagal nuclei, closes the pyloric sphincter, releases hormones secretin and cholecystokinin that inhibit gastric secretion and stomach emptying
 Click here for an animation that helps you understand gastric secretion. Click here for an animation that helps you understand gastric secretion.
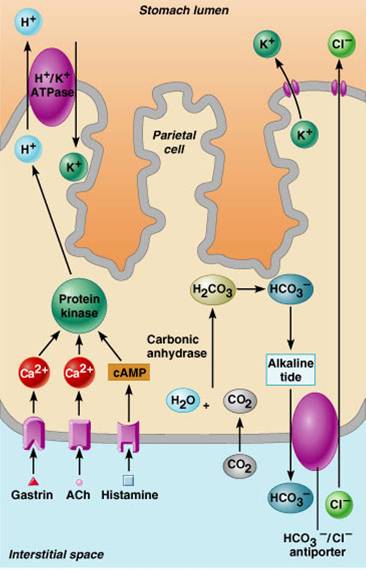
Regulation of HCl Secretion
- Hydrocholoric acid (HCl) secretion is stimulated by:
- Acetylcholine (ACh),
- Histamine
- Gastrin through second messenger systems
- The release of HCl is low if only one of above ligands binds to parietal cell
- The release of HCl is high if all three ligands bind to parietal cells
- Antihistamines block H2 receptors and decrease HCl release
Response of the Stomach to Filling
- Stomach pressure remains constant until about 1L of food is ingested
- Reflex-mediated events include:
- Receptive relaxation – as food travels in the esophagus, stomach muscles relax
- Adaptive relaxation – the stomach dilates in response to gastric filling
Gastric Contractile Activity:
- Peristaltic waves move toward the pylorus at the rate of 3 per minute. This basic electrical rhythm BER) is initiated by pacemaker cells (cells of Cajal).
- Most vigorous peristalsis and mixing occurs near the pylorus
- Chyme is either delivered in small amounts to the duodenum or forced backward into the stomach for further mixing
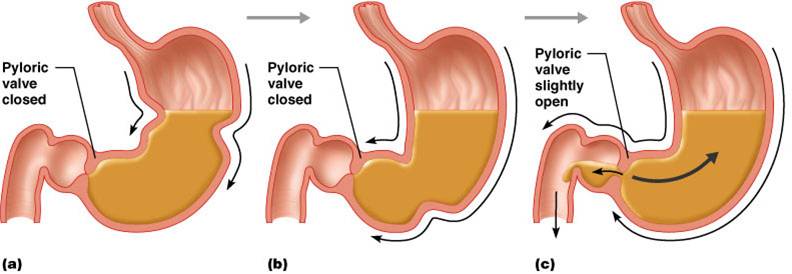
Regulation of Gastric Emptying
2 mechanisms inhibit gastric secretion and duodenal filling:
1. Neural enterogastric reflex
2. Hormonal (enterogastrone) mechanisms:
- Carbohydrate-rich chyme quickly moves through the duodenum
- Fat-laden chyme is digested more slowly causing food to remain in the stomach longer
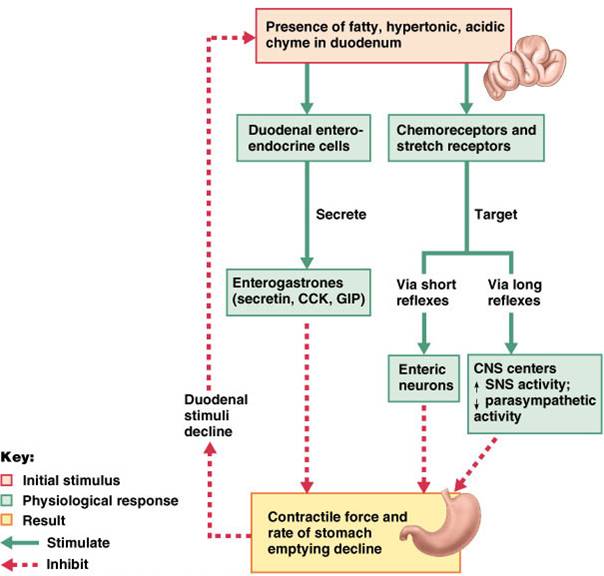
Digestion in Stomach
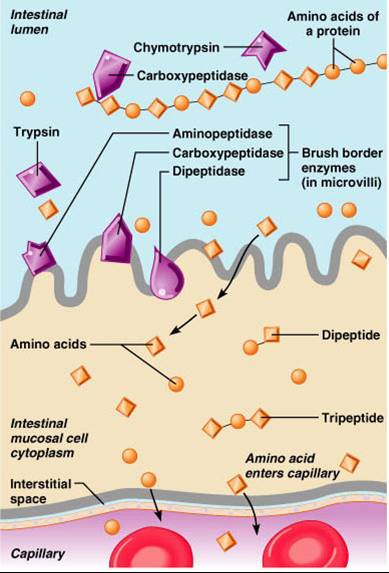
- Preliminary digestion of proteins via pepsin occurs in stomach
- Very little absorption of nutrients occurs
Small Intestine
- Important digestive and absorptive functions
- 3 subdivisions:
- Ileocecal sphincter - transition between small and large intestine
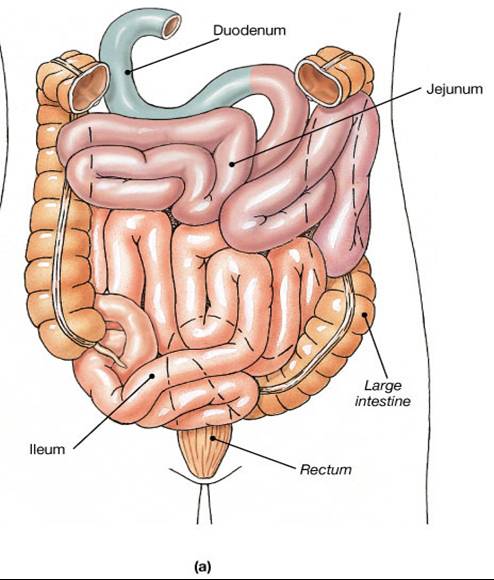
Small Intestine Wall
Structural modifications of the small intestine wall increase surface area
- Plicae circulares: deep circular folds of the mucosa and submucosa
- Villi – fingerlike extensions of the mucosa
- Microvilli –– tiny projections of absorptive mucosal cells’ plasma membranes
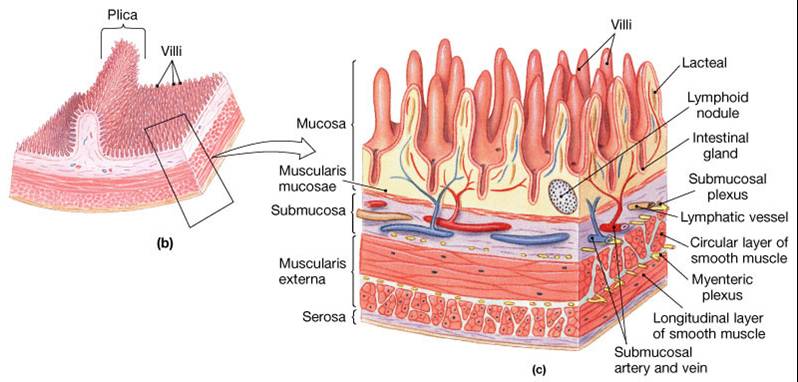
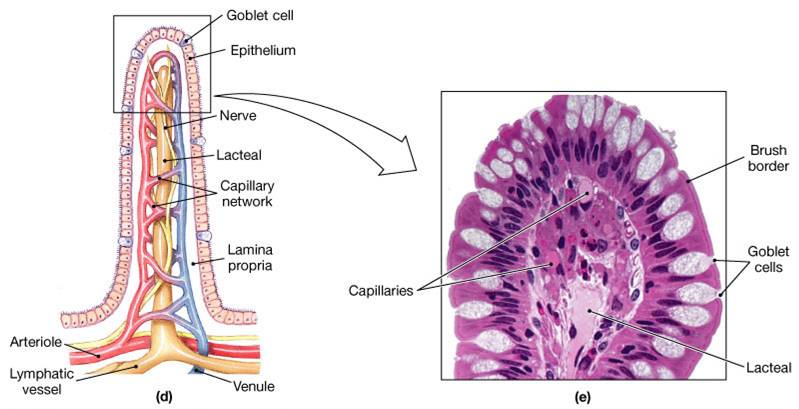
- The epithelium of the mucosa is made up of:
- Absorptive cells and goblet cells
- Enteroendocrine cells
- Interspersed T cells called intraepithelial lymphocytes (IELs)
- Cells of intestinal crypts secrete intestinal juice
- Secreted in response to distension or irritation of the mucosa
- Slightly alkaline and isotonic with blood plasma
- Largely water, enzyme-poor, but contains mucus
Organs that Secrete Substances Into Small Intestine
- Pancreas
- Liver
- Gallbladder
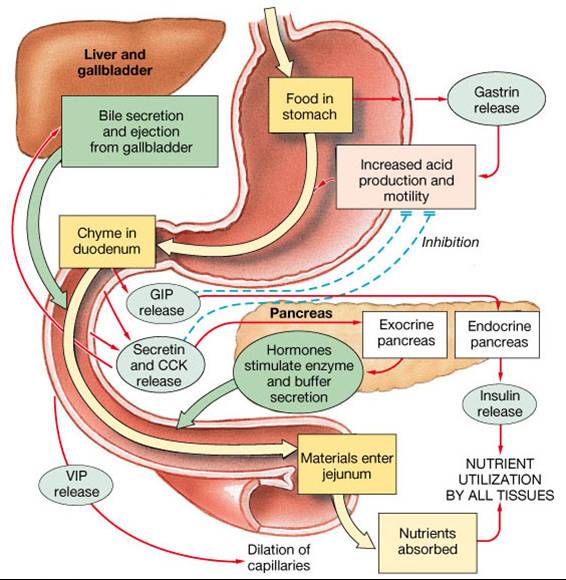
Hormones That Regulate Digestion
Gastrin
- Release is stimulated by expansion of stomach wall by ingested materials; protein and caffein in stomach; and alkaline chyme
- Stimulates secretion of gastric juice (HCl, mucus, and pepsinogen)
Secretin
- Release is stimulated by acidic chyme in the duodenum
- Stimulates pancreatic duct cells to produce large volume of aqueous sodium bicarbonate (NaHCO3) secretion to help neutralize acid in chyme
- Inhibits gastric emptying in order to prevent further acid from entering duodenum until acid already present is neutralized
- Inhibits gastric secretion to reduce amount of acid being produced
- Stimulates liver to secrete NaHCO3 rich bile which assists in neutralization process
- Along with CCK, is trophic to exocrine pancreas
Cholecystokinin (CCK)
- Release is stimulated by triglycerides, fatty acids, and amino acids in the duodenum
- Stimulates pancreatic acinar cells to increase secretion of pancreatic enzymes
- Causes contraction of gallbladder
- inhibits gastric motility and secretion
- Stimulates relaxation of muscle to open hepatopancreatic sphincter
- Along with secretin, is trophic to exocrine pancreas
- Implicated in long-term adaptive changes in proportion of pancreatic enzymes in response to prolonged diet changes
- Important regulator of food intake
Gatric Inhibitory Polypeptide (GIP)
- Stimulates release of insulin,
- inhibits gastric secretion and motility
Functions of Glands of the Duodenum:
- Moisten chyme
- Help buffer acids
- Naintain digestive material in solution
Liver
- Largest gland in the body,
- Performs metabolic and hematological regulation
- Produces and secretes bile
- Produces proteins involved in blood coagulation
- Stores absorbed productions of digestion (such as carbohydrates, fats, vitamins, and iron)
- Detoxifies poisons to make them less toxic and more easily eliminated from the body
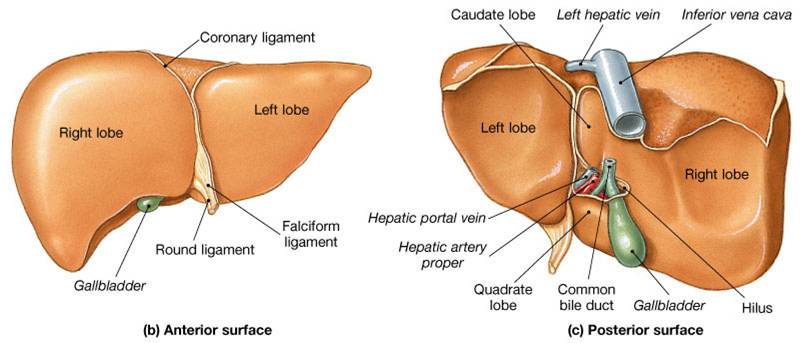
 Click here for an animation that reviews the anatomy of the liver, the functions of the liver, and the structure of liver lobules. Click here for an animation that reviews the anatomy of the liver, the functions of the liver, and the structure of liver lobules.
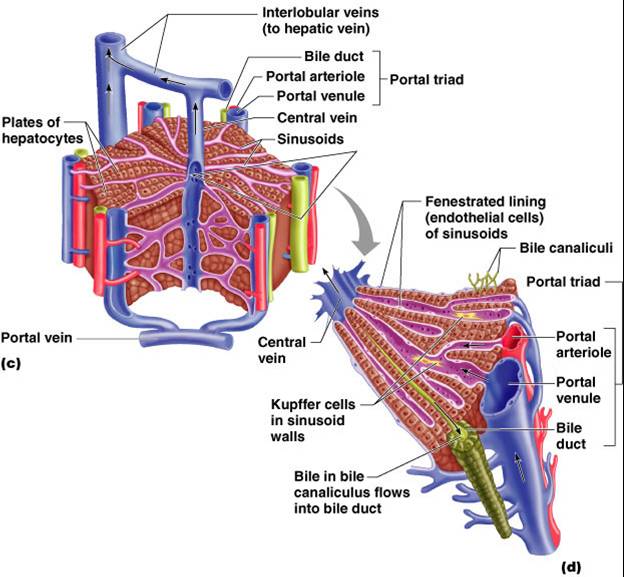
Liver Lobules
- Are hexagonal-shaped structures
- Are the structural and functional units of the liver
- Are composed of hepatocytes
- Hepatocyte functions include:
- Production of bile
- Processing bloodborne nutrients
- Storage of fat-soluble vitamins
- Detoxification
- Secreted bile flows between hepatocytes toward the bile ducts in the portal triads (formed by branches of the hepatic artery, hepatic portal veins, and bile duct)
Composition of Bile
- Is a yellow-green, alkaline solution
- Contains bile salts, bile pigments, cholesterol, neutral fats, phospholipids, and electrolytes
- Bile salts are cholesterol derivatives that:
- emulsify fat,
- facilitate fat and cholesterol absorption,
- help solubilize cholesterol
- Chief bile pigment is bilirubin, a waste product of heme
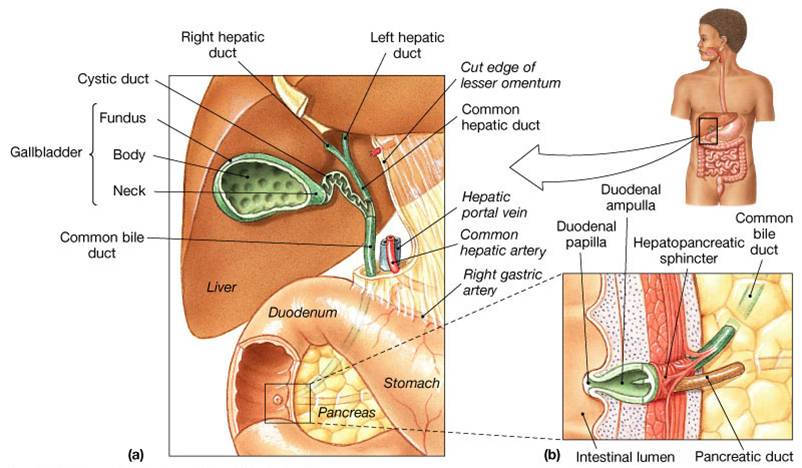
Gallbladder
- Is a thin-walled, green muscular sac on the ventral surface of the liver
- Stores and concentrates bile by absorbing its water and ions
- Releases bile via the cystic duct, which flows into the bile duct
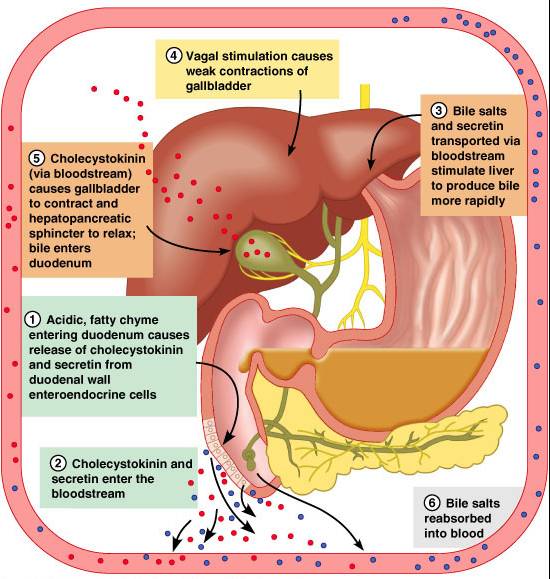
Regulation of Bile Release
- Acidic, fatty chyme causes the duodenum to release cholecystokinin (CCK) and secretin into the bloodstream
- Bile salts and secretin transported in blood then stimulate the liver to produce bile
- Vagal stimulation causes weak contractions of the gallbladder
- Cholecystokinin causes the gallbladder to contract, the hepatopancreatic sphincter to relax; as a result, bile enters the duodenum
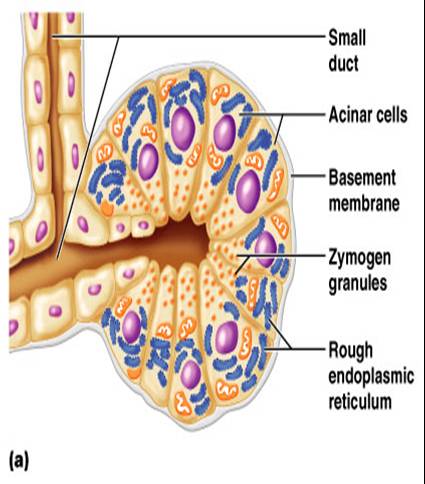
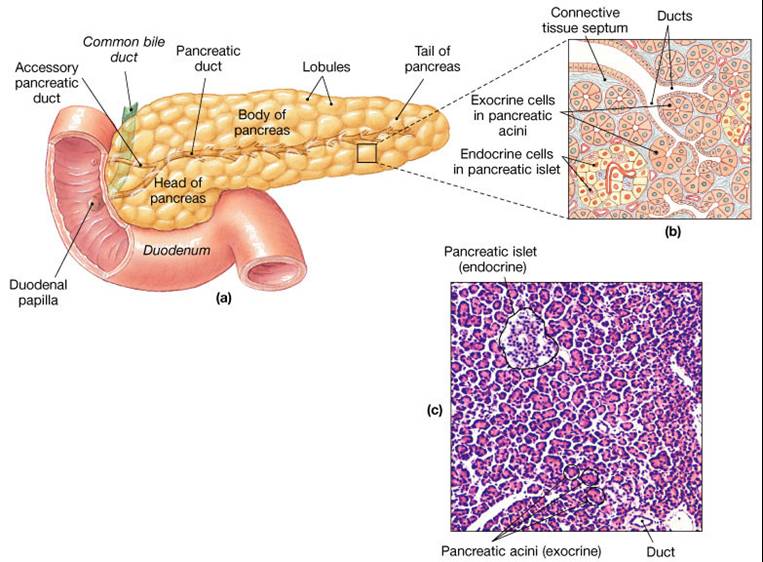
Pancreas
2 separate functions:
1. Endocrine functions
- secretes insulin and glucagons
2. Exocrine functions
- secretes pancreatic juice into small intestine which breaks down all categories of foodstuff
- acini (clusters of secretory cells) contain zymogen granules with digestive enzymes
Composition of Pancreatic Juice
- Is a water solution of enzymes and electrolytes (primarily HCO3+)
- Neutralizes acid chyme to provide optimal environment for pancreatic enzymes
- Enzymes are released in inactive form and activated in the duodenum
- Trypsinogen is activated to trypsin
- Procarboxypeptidase is activated to carboxypeptidase
- Active enzymes secreted: amylase, lipases, and nucleases; these enzymes require ions or bile for optimal activity
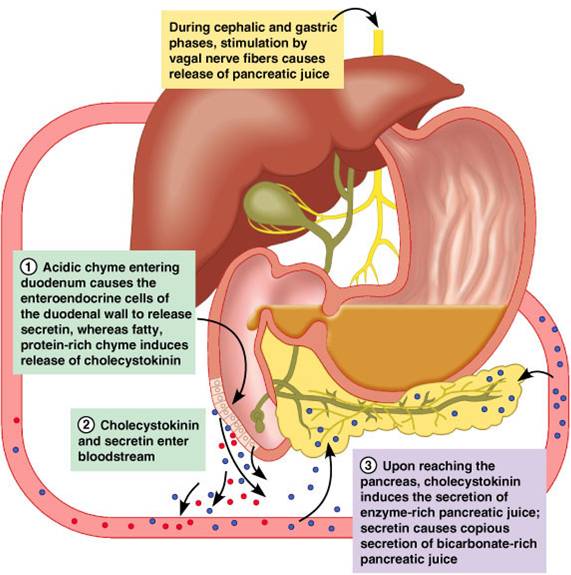
Regulation of Pancreatic Juice
- Secretin and CCK are released when fatty or acidic chyme enters the duodenum
- CCK and secretin enter the bloodstream
- Upon reaching the pancreas, CCK induces the secretion of enzyme-rich pancreatic juice
- Secretin causes secretion of bicarbonate-rich pancreatic juice. Vagal stimulation also causes release of pancreatic juice
Digestion in the Small Intestine
- As chyme enters the duodenum, carbohydrates and proteins are only partially digested, no fat digestion has taken place
- Digestion continues in the small intestine:
- Chyme is released slowly into the duodenum.
- Because chyme is hypertonic and has low pH, mixing is required for proper digestion
- Required substances needed are supplied by the liver
Absorption of Nutrients Occurs in the Small Intestine
- The most common motion of the small intestine is segmentation. It is initiated by intrinsic pacemaker cells (Cajal cells)
- Segmentation moves contents steadily toward the ileocecal valve
- After nutrients have been absorbed, peristalsis begins with each wave starting distal to the previous; meal remnants, bacteria, mucosal cells, and debris are moved into the large intestine
Control of Intestinal Motility
- Local enteric neurons of the GI tract coordinate intestinal motility
- Cholinergic neurons cause contraction and shortening of the circular muscle layer, shortening of longitudinal muscle, distension of the intestine
- Other impulses relax the circular muscle
- The gastroileal reflex and gastrin relax the ileocecal sphincter and allow chyme to pass into the large intestine
Large Intestine
Functions:
- Reabsorb water and compact material into feces, absorb vitamins produced by bacteria
- Store fecal matter prior to defecation
- Other than digestion of enteric bacteria, no further digestion takes place
- Vitamins, water, and electrolytes are reclaimed
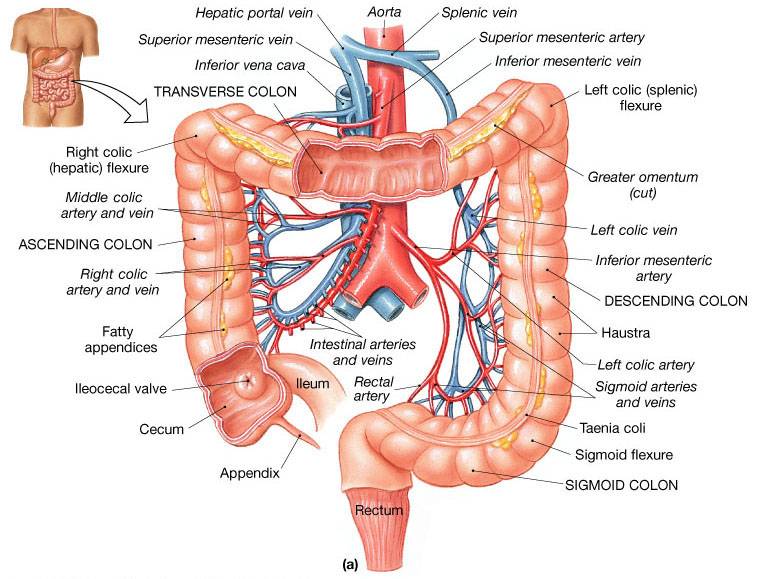
Motility of the Large Intestine
- Haustral contractions - slow segmenting movements that move the contents of the colon
- Haustra sequentially contract as they are stimulated by distension
- Haustral contractions initiatei peristalsis that forces contents toward the rectum
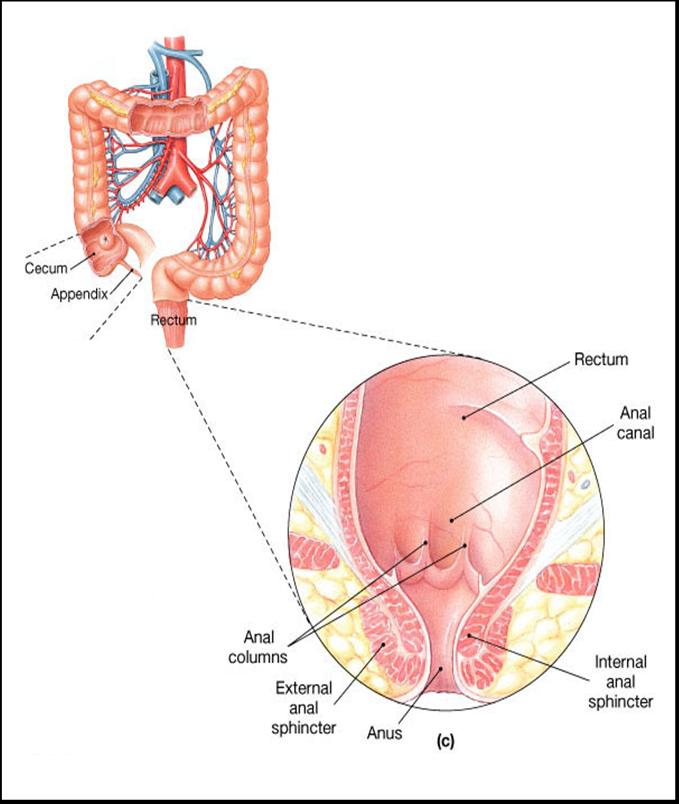
Rectum
- Is the l ast portion of the digestive tract
- It terminates at the anal canal
- Defecation reflex is triggered by distention of rectal walls by feces:
- Defecatin reflex stimulates contraction of the rectal walls, relaxes the internal anal sphincter
- Voluntary signals stimulate relaxation of the external anal sphincter and defecation occurs
Chemical Digestion and Absorption of Carbohydrates
- Carbohydrates are broken down into monosaccharides
- Digestion of carbohydrates begins in the mouth by the enzyme salivary amylase found in saliva
- Pancreatic enzymes and brush border enzymes then break down the carbohydrates into monosaccharides
- Absorption of monosaccharides occurs across the intestinal epithelia via cotransport with Na+ons, and facilitated diffusion; the monosaccharides enter the capillary bed in the villi
- Monosaccharides are transported to the liver via the hepatic portal vein
|