Reproductive System
|
Content
Primary Reproductive Organs (gonads)
Male Reproductive System
Male Sexual Response
Hormonal Regulation of Spermiogenesis
Testosterone
Female Reproductive System
Menstrual Cycle
Stages of Pregnancy and Development
Primary Reproductive Organs (gonads)
The primary reproductive organs are the organs responsible for
- producing the egg and sperm cells (gametes),
- producing hormones that function in the maturation of the reproductive system
- the development of sexual characteristics
- regulating the normal physiology of the reproductive system
Male primary reproductive organs: testes
Female primary reproductive organs: ovaries
Accessory Reproductive Organs
All other organs in the reproductive system are considered secondary (or accessory) reproductive organs. These are the ducts, and glands that transport and sustain the gametes and nurture the developing offspring.
Sex Hormones
- Males: androgens (ex: testosterone)
- Females: estrogens and progesterone
- Function:
- -Development of the reproductive organs
- -Function of the reproductive organs
- -Sexual behavior and drives
- -Growth and development of many other organs and tissues
Sex Hormones of the Anterior Pituitary Gland (Adenohypophysis)
Follicle stimulating hormone (FSH)
Stimulates follicle development and estrogen secretion in females and sperm production in males
Luteinizing hormone (LH)
Causes ovulation and progestin production in females and androgen production in males
Prolactin (PL)
Stimulates the development of mammary glands and milk production
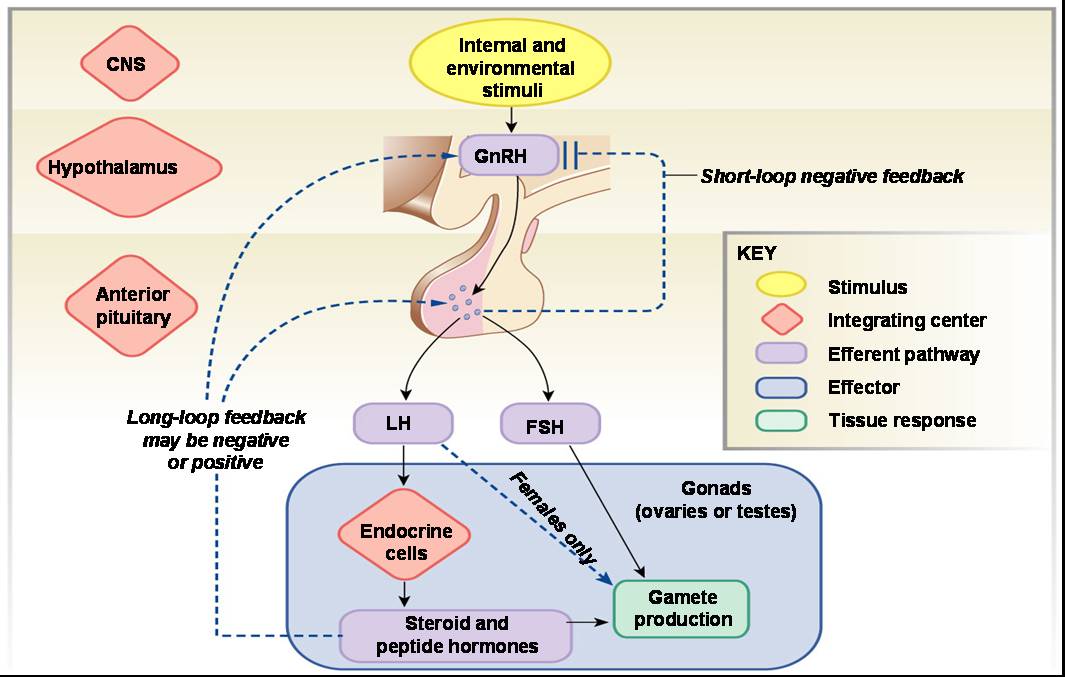
Click here for an animation that provides an example of positive and negative feedback control of the reproductive hormones.
This animation is followed by practice questions. Click here for even more practice questions.
Male Reproductive System
Testes (2)
- Produce sperm and lie within the scrotum
- Sperm are delivered to the exterior through a system of ducts: epididymis, ductus deferens, ejaculatory duct, and the urethra
- Seminiferous tubules within the testes produce the sperm
- Surrounding the seminiferous tubules are interstitial (Leydig) cells that produce androgens
- Epididymis functions to mature and store sperm cells (at least 20 days)
- Spermatic cord encloses PNS and SNS nerve fibers, blood vessels, and lymphatics that supply the testes
- The accessory sex glands empty their secretions into the ducts during ejaculation
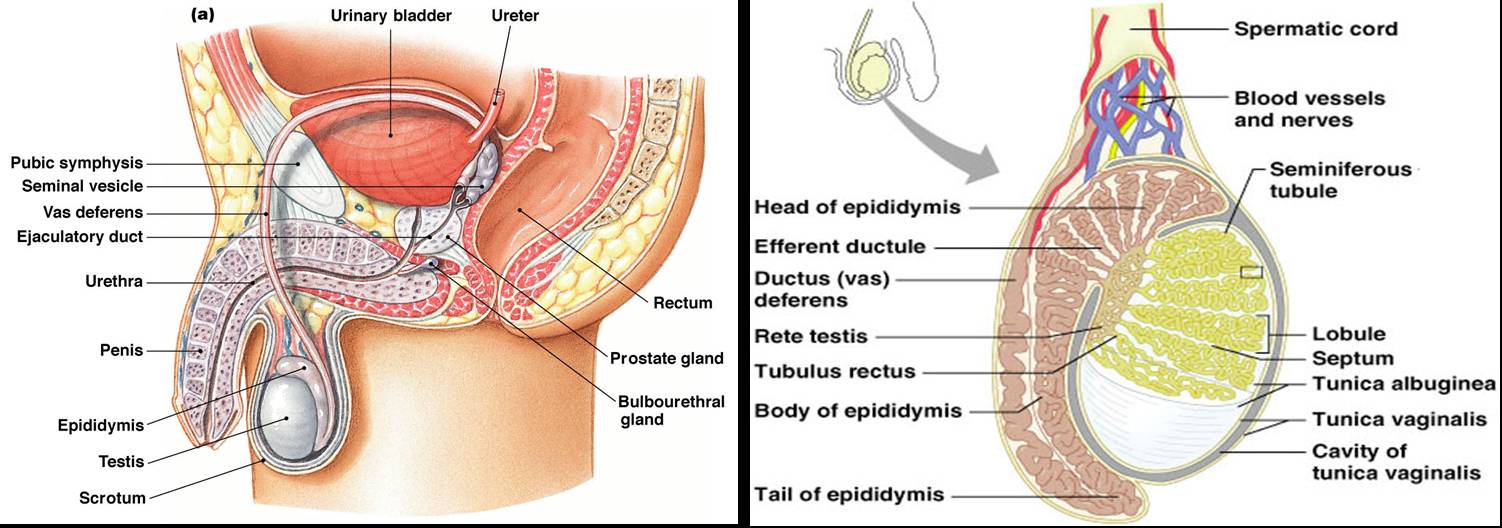
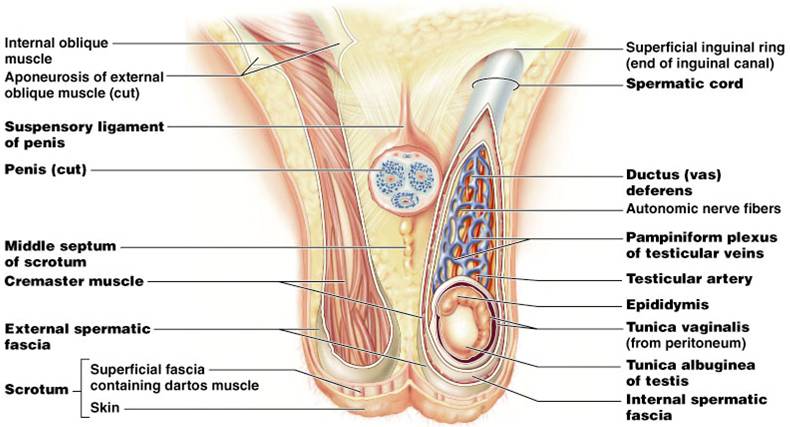
Scrota (2) (scrotum = singular)
- Each of the 2 scrota contains a testicle that hangs outside the abdominopelvic cavity.
- Its external positioning keeps the testes 3°C lower than core body temperature (needed for sperm production)
- Intrascrotal temperature is kept constant by two sets of muscles:
-dartos – smooth muscle that wrinkles scrotal skin
-cremaster – bands of skeletal muscle that elevate the testes
|
Penis
- Urethra conveys both urine and semen (at different times!)
- Made of cylindrical bodies of erectile tissue (spongy network of connective tissue and smooth muscle riddled with vascular spaces):
-corpus spongiosum (1)
-corpora cavernosa (2)
- During sexual excitement, the erectile tissue fills with blood causing the penis to enlarge and become rigid (erection)
|
 # # |
Semen
- Mixture of sperm and seminal fluid
- Is milky white, and sticky
- Provides a transport medium
- Provides nutrients (fructose)
- Protects and activates sperm
- Facilitates movement of sperm
- Prostaglandins in semen:
-Decrease the viscosity of mucus in the cervix
-Stimulate reverse peristalsis in the uterus, facilitates movement through female reproductive tract
-Suppress immune response of female
- The hormone relaxin enhances sperm motility
- The relative alkalinity of semen neutralizes the acid environment found in the male urethra and female vagina
- Seminalplasmin – antibiotic chemical that destroys certain bacteria
- Clotting factors coagulate semen immediately after ejaculation, then fibrinolysin liquefies the sticky mass
- Only 2-5 ml of semen are ejaculated, but it contains 50-130 million sperm/ml
Accessory Glands
Accessory glands secrete various fluids that make up the seminal fluid that, together with sperm, make up the semen.
Seminal Vesicles (2)
- Secrete 60% of the volume of semen
- Secrete viscous alkaline fluid containing fructose, ascorbic acid, coagulating enzyme (vesiculase), and prostaglandins
- Join the ductus deferens to form the ejaculatory duct where sperm and seminal fluid mix
Prostate Gland (1)
- Secretes about 30% of volume of semen
- Gland that encircles part of the urethra inferior to the bladder
- Secretes milky, slightly acid fluid, which contains citrate and enzymes
- Plays a role in the activation of sperm
Bulbourethral Glands (2)
- Secrete about 10% of volume of semen
- Are pea-sized glands inferior to the prostate
- Produce thick, clear mucus prior to ejaculation that neutralizes traces of acidic urine in the urethra
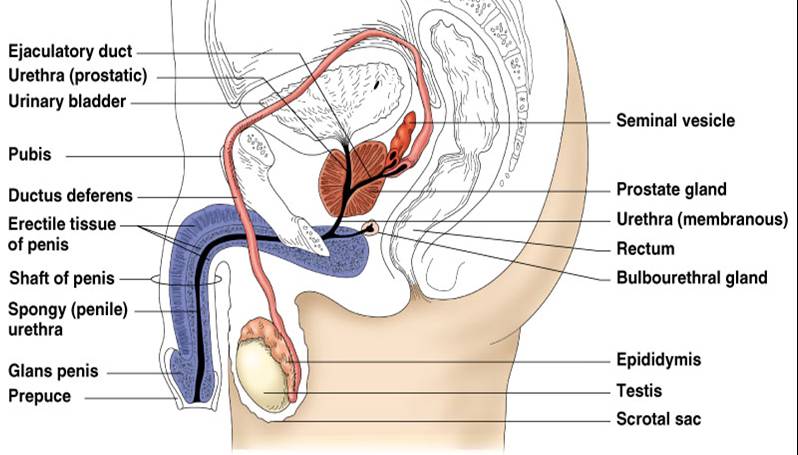
Click here for an animation that provides an overview of the organs of the male reproductive system.
|
Male Sexual Response
Erection
- An erection is the enlargement and stiffening of the penis from engorgement of erectile tissue with blood
- Erections are initiated by sexual stimuli including:
- -Touch and mechanical stimulation of the penis
- -Erotic sights, sounds, and smells
- Erections can be induced or inhibited solely by emotional or higher mental activity
- Mechanism:
- During sexual arousal, a parasympathetic reflex promotes the release of nitric oxide
- Nitric oxide causes erectile tissue to fill with blood
- Expansion of the corpora cavernosa compresses the drainage veins of the penis which retards blood outflow and maintains engorgement
- Impotence – inability to attain erection
Ejaculation
- The corpus spongiosum functions in keeping the urethra open during ejaculation (release of semen)
- At ejaculation, sympathetic nerves serving the genital organs cause:
- Reproductive ducts and accessory organs to contract and empty their contents
- Bladder sphincter muscle to constrict, preventing the expulsion of urine
- Epididymis, seminal vesicles, prostate gland and bulbospongiosus muscles to rhythmically contract, propelling the semen (about 3-5 ml) through the urethra
|
Path of Sperm During Ejaculation
- From seminiferous tubules, the sperm enter the epididymis
- Upon ejaculation the epididymis contracts, expelling sperm into the ductus deferens (also called vas deferens)
- Ductus deferens merges with the duct of the seminal vesicle to form the ejaculatory duct
- From the ejaculatory duct, sperm enter and then leave the urethra
- Vasectomy – cutting and ligating the ductus deferens, which is a nearly 100% effective form of birth control
|
Spermatogenesis
Spermatogenesis is the development of sperm cells that occurs in the seminiferous tubules of the testes. The process begins at puberty and continues throughout adult life. Male sex hormones regulate this process. Cells making up the walls of seminiferous tubules are in various stages of cell division.
The stages in spermatogenesis can be summarized as follows:
spermatogonium ---> primary spermatocyte ---> secondary spermatocyte ---> early spermatids ----> late spermatids ---> sperm cells
Click here for an animation on spermatogenesis.
The animation is followed by practice questions. Click here for even more practice questions.
|
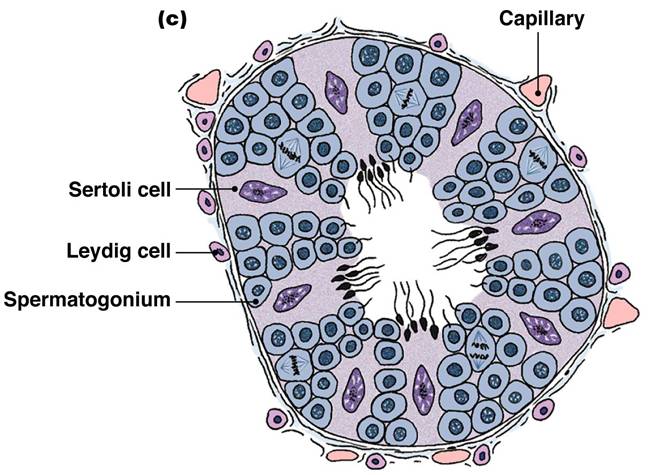 |
1. Mitosis of Spermatogonia
- The spermatogonium is a stem cell found in the outer wall of the seminiferous tubules within the testes. They are in contact with the epithelial basal lamina.
- Each spermatogonium has two sets of chromosomes (one maternal, one paternal) and is said to be diploid (2n chromosomal number). Thus, each spermatogonium has 23 pairs of homologous chromosomes or a total of 46 chromosomes.
- A spermatogonium undergo mitosis, which results in 2 new cells-type A and type B.
- Type A cells remain at the basement membrane and maintain the germ line
- Type B cells move toward the lumen and become primary spermatocytes
- Thus, we say mitosis of spermatogonia forms spermatocytes.
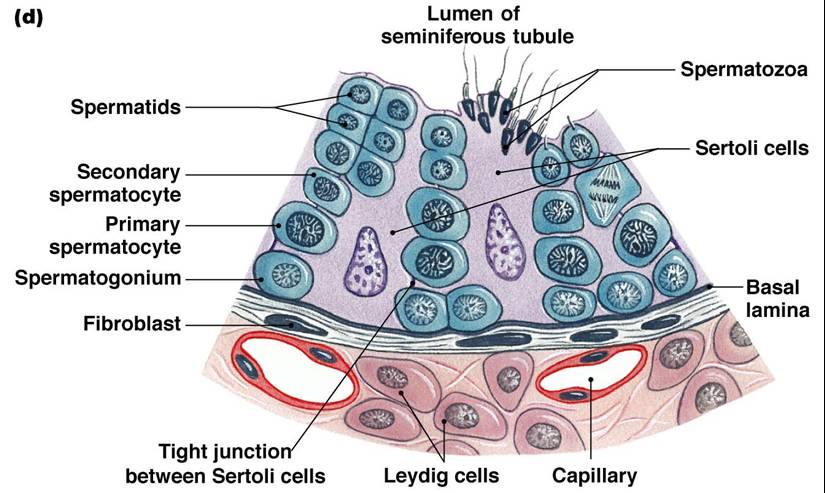
2. Meiosis of Spermatocytes
- A primary spermatocyte undergo meiosis I, forming two secondary spermatocytes.
- Secondary spermatocytes undergo meiosis II and their daughter cells are called spermatids.
- Spermatids are small round cells seen close to the lumen of the tubule.
- Spermatids only have 23 chromosomes and are said to be haploid (n chromosomal number).
- Gamete formation is by meiosis, in which the number of chromosomes is halved (from 2n to n).
- Thus, we say meiosis of spermatocytes forms spermatids.
Click here for an animation that compares mitosis and meiosis.
The animation is followed by practice questions.
|
 |
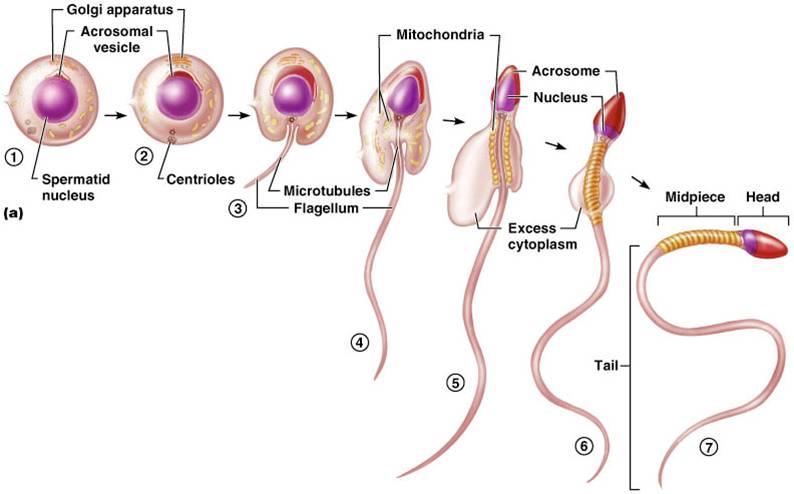
3. Spermiogenesis
Spermiogenesis is the process in which spermatids develop into sperm. The spermatids lose excess cytoplasm and form a tail, becoming motile sperm
Sperm
Sperm have 3 major regions
- Head – contains DNA and hydrolytic enzymes that allow the sperm to penetrate and enter the egg
- Midpiece – contains mitochondria spiraled around filaments
- Tail – a typical flagellum produced by a centriole
|
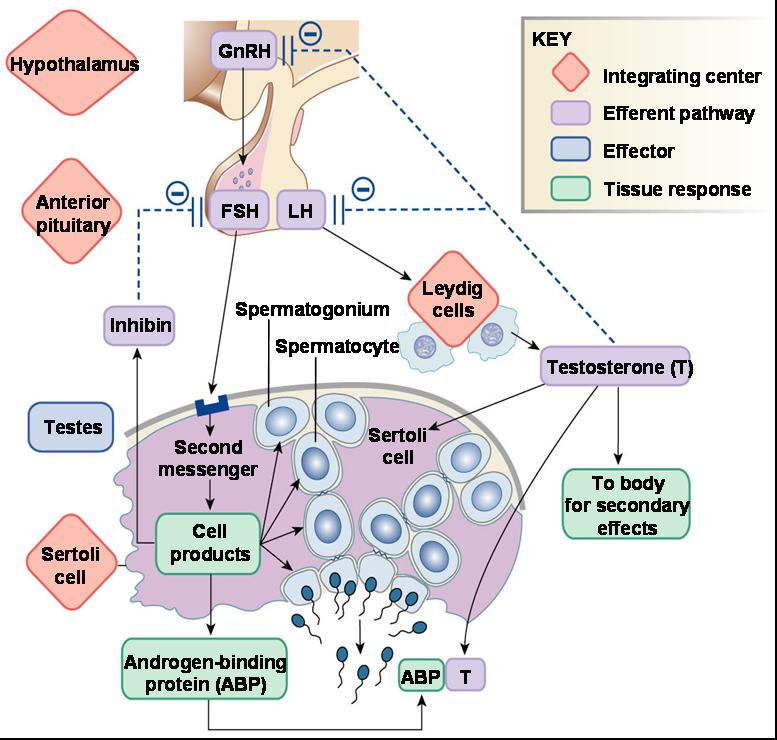
Hormonal Regulation of Spermiogenesis
- The hypothalamus releases gonadotropin-releasing hormone (GnRH)
- GnRH stimulates the anterior pituitary to secrete FSH and LH
- FSH causes sustentacular (Sertoli) cells to release androgen-binding protein (ABP)
- LH stimulates interstitial (Leydig) cells to release testosterone
- ABP binding of testosterone enhances spermatogenesis
Feedback inhibition on the hypothalamus and pituitary results from rising levels of testosterone and increased production of inhibin |
|
 |
Testosterone
- Synthesized from cholesterol
- Necessary for fetal development of male external genitalia
- Increased levels of testosterone at puberty are responsible for further growth of male genitalia and for the development and maintenance of male secondary sex characteristics
- Stimulates protein synthesis and accounts for the greater muscular development of the male
- Is the basis of libido in both males and females
- Stimulates development of male secondary sexual characteristics including:
- -Appearance of pubic, axillary, and facial hair
- -Enhanced growth of the chest and deepening of the voice
- -Skin thickens and becomes oily
- -Bones grow and increase in density
- -Skeletal muscles increase in size and mass
Female Reproductive System
Ovaries
- Are the primary female reproductive organs
- Produce female gametes (ova)
- Secrete female sex hormones (estrogen and progesterone)
- Have ovarian follicles embedded in the ovary cortex are ovarian follicles; each follicle consists of an immature egg called an oocyte
Accessory Organs
- Uterine tubes (Fallopian tubes)
- Uterus
- Vagina
- Internal genitalia – ovaries and the internal ducts
- External genitalia – external sex organs
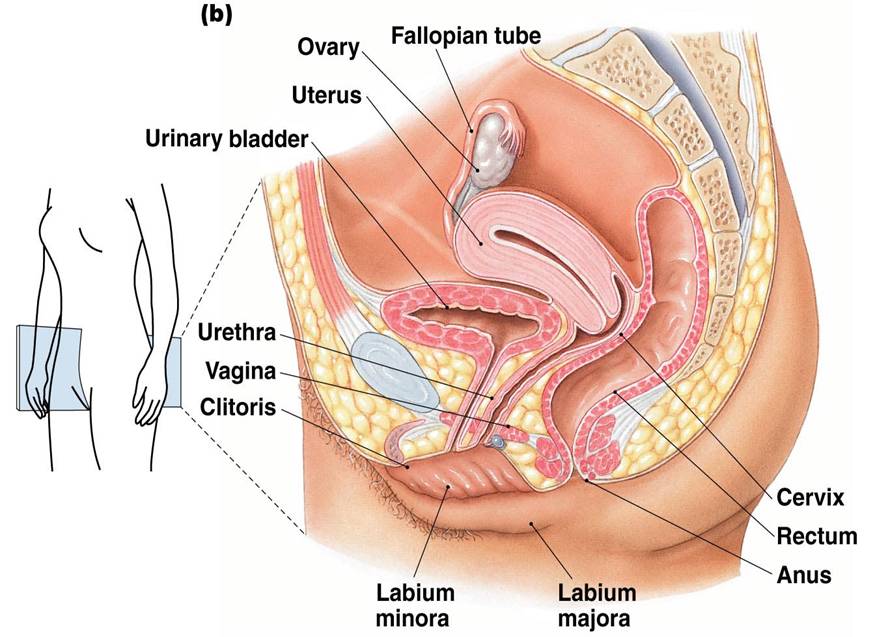
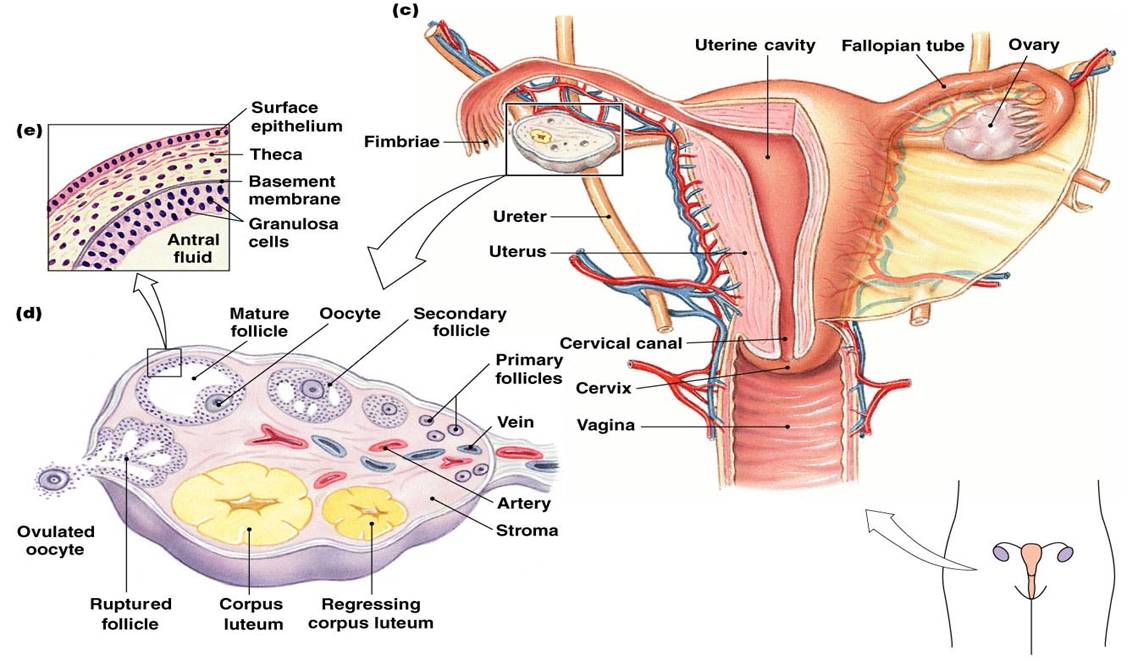
Ovarian Cycle
- Primordial follicle – one layer of squamouslike follicle cells surrounds the oocyte
- Primary follicle – two or more layers of cuboidal granulosa cells enclose the oocyte
- Graafian follicle – secondary follicle at its most mature stage that bulges from the surface of the ovary
- Ovulation – ejection of the oocyte from the ripening follicle
- Corpus luteum – ruptured follicle after ovulation
Click here for an animation on the development of a primordial follicle during the ovarian cycle.
This animation is followed by practice questions.
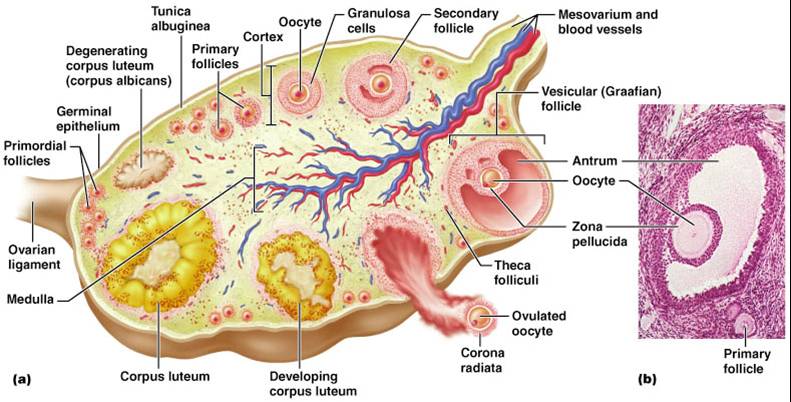
Uterine Tubes (Fallopian Tubes)
- Receive the ovulated oocyte and provide a site for fertilization
- Have no contact with the ovaries (the ovulated oocyte is released into the peritoneal cavity)
- The beating cilia on the fimbriae create currents to carry the oocyte into the uterine tube
- The oocyte is carried toward the uterus by peristalsis and ciliary action
|
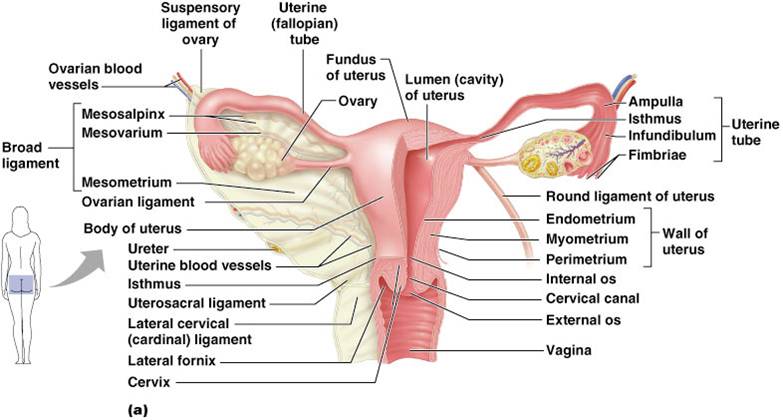
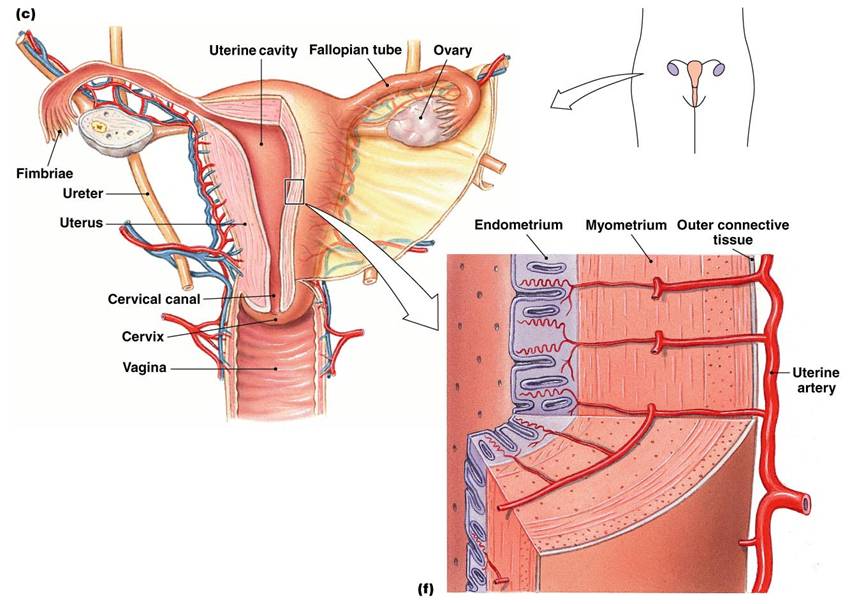
Uterus
- Is a hollow, thick-walled organ that consists of
Body – major portion of the uterus
Fundus – rounded region superior to the entrance of the uterine tubes
Cervix – narrow outlet that protrudes into the vagina
- Functions of the uterus
Receives, retains, and nourishes the fertilized egg
- Uterine wall is composed of 3 layers:
1. Perimetrium – outermost serous layer; the visceral peritoneum
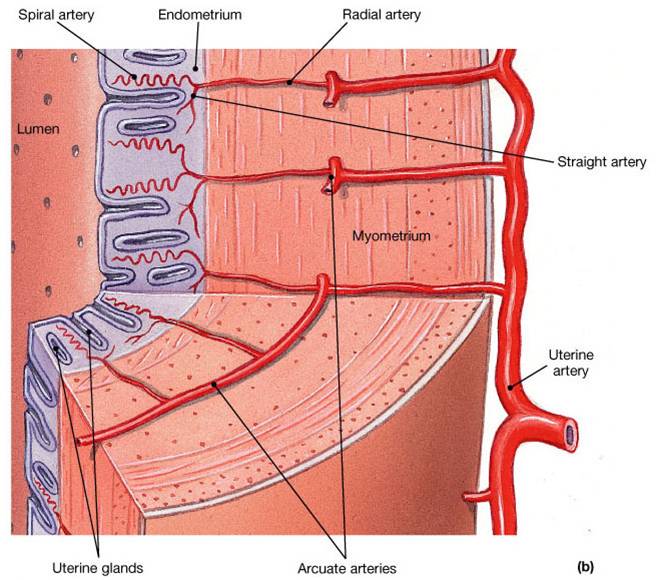
2. Myometrium – middle layer; interlacing layers of smooth muscle
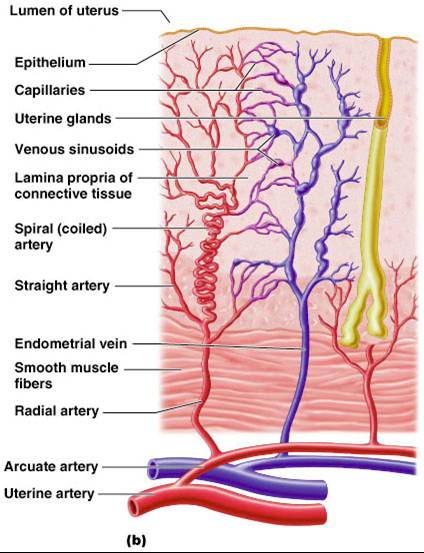
3. Endometrium – mucosal lining of the uterine cavity. Inner layer allows for implantation of a fertilized egg. Sloughs off if no pregnancy occurs (menses). Has numerous uterine glands that change in length as the endometrial thickness changes
|
 |
 |
Vagina
- Is a thin-walled tube lying between the bladder and the rectumExtends from the cervix to the exterior of the body
- The urethra is embedded in the anterior wall
- Provides a passageway for birth, menstrual flow
- Organ of copulation - receives the penis during sexual intercourse
- Vaginal mucosa has NO glands, so lubrication is provided by cervical mucus glands / vestibular glands (outside vagina)
- pH of the vagina in menarchal (reproductive) women is acidic
- Maintained by glycogen stores that are used by resident normal flora (bacteria)
- Bacteria produce lactic acid as waste product, making the vagina acidic
- Low pH is hostile to sperm
- High pH of seminal secretions aid to neutralize the acidic pH of the vagina and enhance survival of sperm.
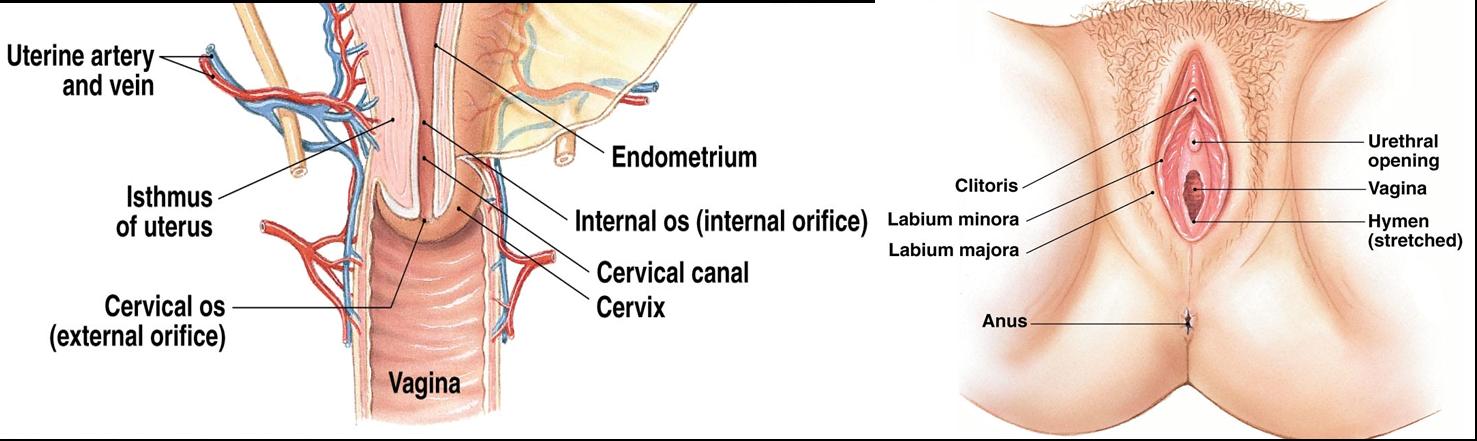
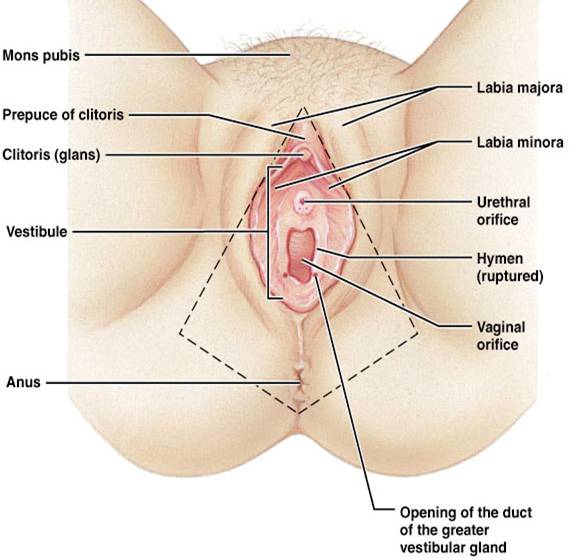
Vulva (part of the external genitalia)
- Mons pubis - mound of fatty tissue overlying the pubic symphysis (pubic bone)
- Labia majora - outer folds of skin contains fat, sudoriferous and sebaceous glands, covered with pubic hair (homologous to scrotum)
- Labia minora - inner folds of skin containing sebaceous glands and nerve endings that provide stimulation
- Clitoris - cylindrical mass of erectile tissue covered by a layer of skin called the prepuce (homologous to penis)
- Vestibule - cleft between the labia minora includes the urethral orifice, vaginal orifice and vestibular glands that produce lubricants during sexual intercourse.
Mammary Glands
- Made of modified sweat glands consisting of 15-25 lobes that radiate around and open at the nipple.
- Lobes contain glandular alveoli that produce milk in lactating women
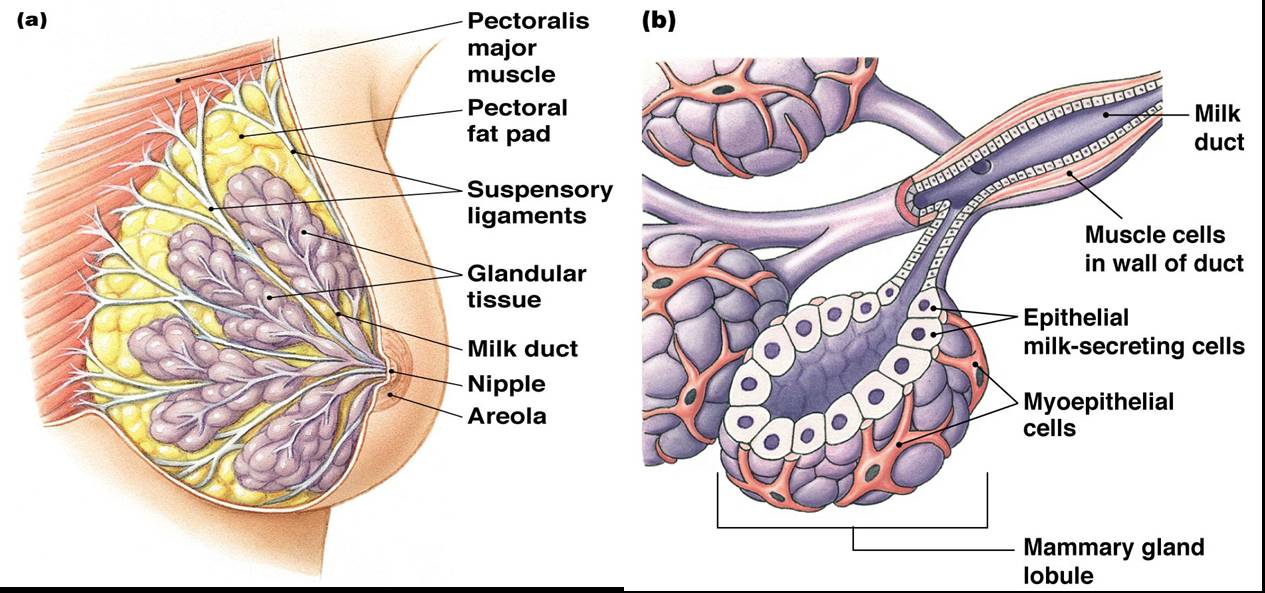
Click here for an animation that provides an overview of the female reproductive organs.
|
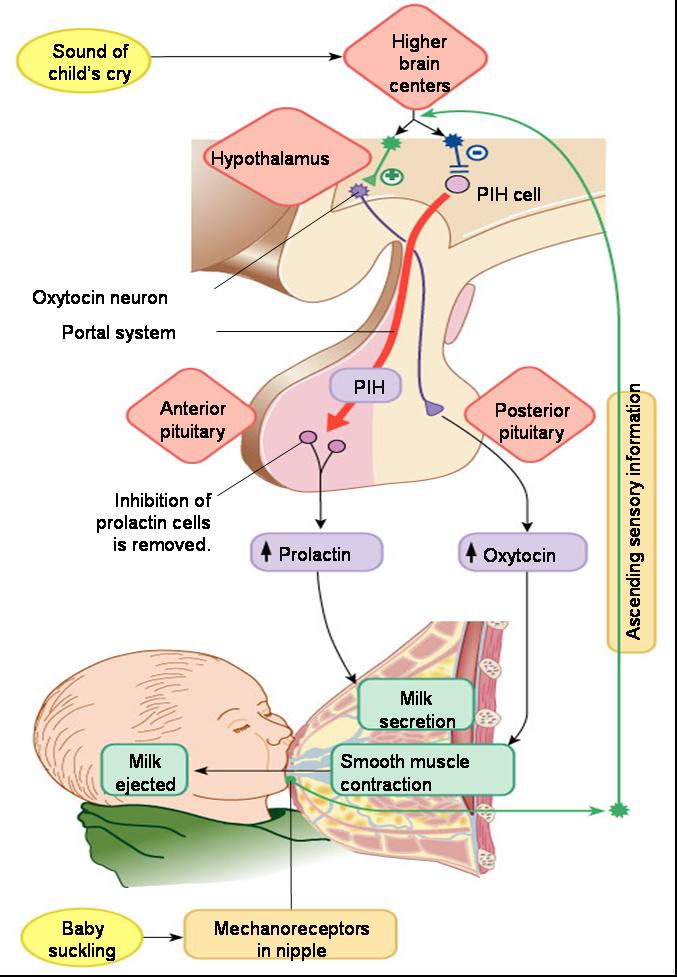
Hormonal Control of Lactation (milk production and release)
- Prolactin-inhibiting hormone (PIH)
- Prolactin - stimulates milk production
- Oxytocin – stimulates milk release “expressed”
- Suckling - inhibits PIH
|
 |
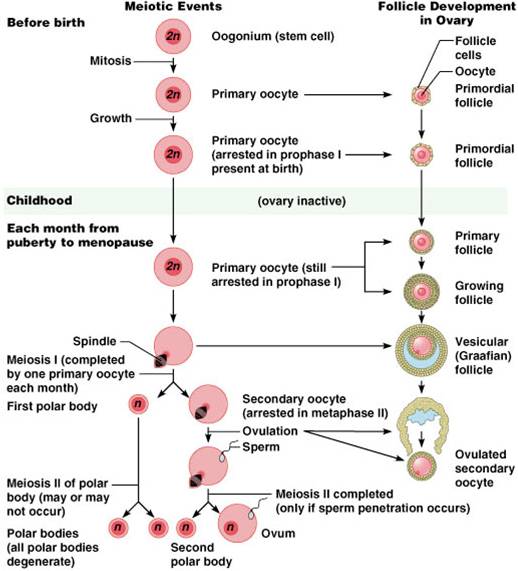
Oogenesis
- Production of female sex cells by meiosis
During fetal period
- Oogonia (2n ovarian stem cells) multiply by mitosis and store nutrients
- Primordial follicles appear as oogonia are transformed into primary oocytes
- Primary oocytes begin meiosis but stall in prophase I
During childhood the ovaries are inactive
From puberty
- Each month one activated primary oocyte completes meiosis one to produce two haploid cells
- The first polar body
- The secondary oocyte
- The secondary oocyte arrests in metaphase II and is ovulated
- If penetrated by sperm the second oocyte completes meiosis II, yielding:
- One large ovum (the functional gamete)
- A tiny second polar body
|
 |
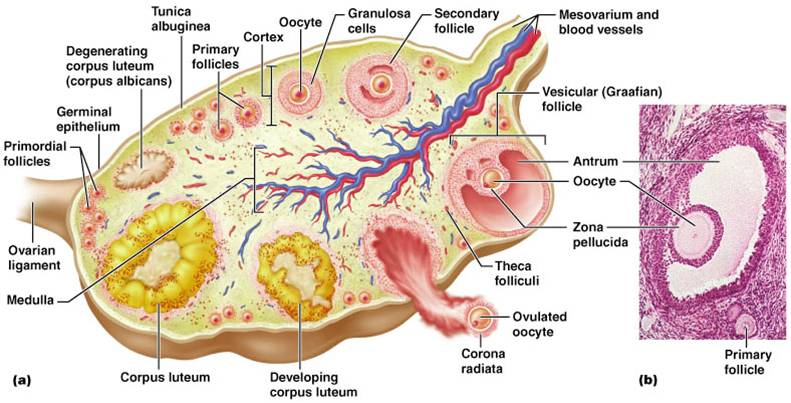
Ovarian Cycle
- Is a Monthly series of events associated with the maturation of an egg
- There are 3 phases:
1. Follicular Phase
- Period of follicle growth (days 1–14)
- The primordial follicle, directed by the oocyte, becomes a primary follicle
- The primary follicle becomes a secondary follicle
- Ttheca folliculi and granulosa cells produce estrogens
- The secondary follicle becomes a mature vesicular follicle (Graafian follicle)
2. Ovulation
- Occurs midcycle
- Occurs when the ovary wall ruptures and expels the secondary oocyte
- Mittelschmerz – a twinge of pain sometimes felt at ovulation
- 1-2% of ovulations release more than one secondary oocyte, which if fertilized, results in fraternal twins
3. Luteal Phase
- After ovulation, the ruptured follicle collapses, granulosa cells enlarge, and along with internal thecal cells, form the corpus luteum.
- The corpus luteum secretes progesterone and estrogen
- If pregnancy does not occur, the corpus luteum degenerates in 10 days, leaving a scar (corpus albicans)
- If pregnancy does occur, the corpus luteum produces hormones until the placenta takes over that role (at about 3 months)
Establishing the Ovarian Cycle
- During childhood: ovaries grow and secrete small amounts of estrogens that inhibit the hypothalamic release of GnRH
- As puberty nears: GnRH is released; FSH and LH are released by the pituitary, which act on the ovaries; these events continue until an adult cyclic pattern is achieved and menarche occurs
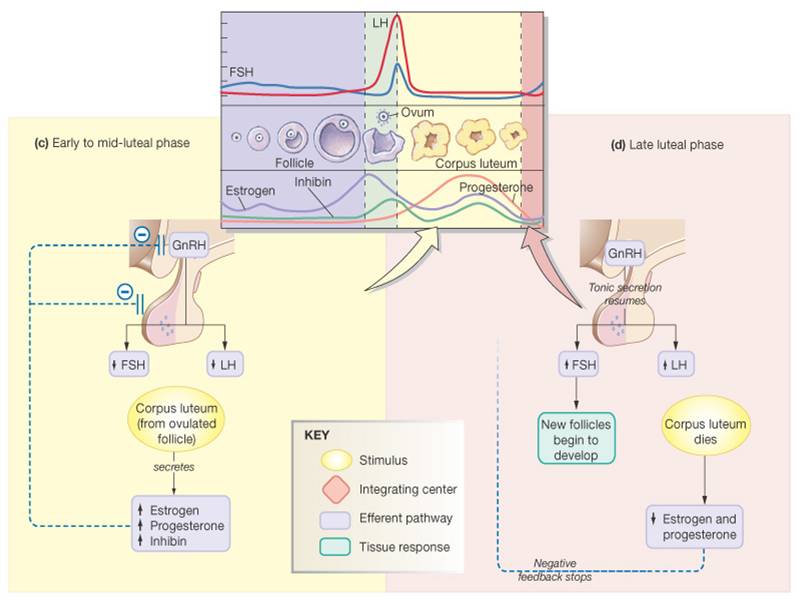
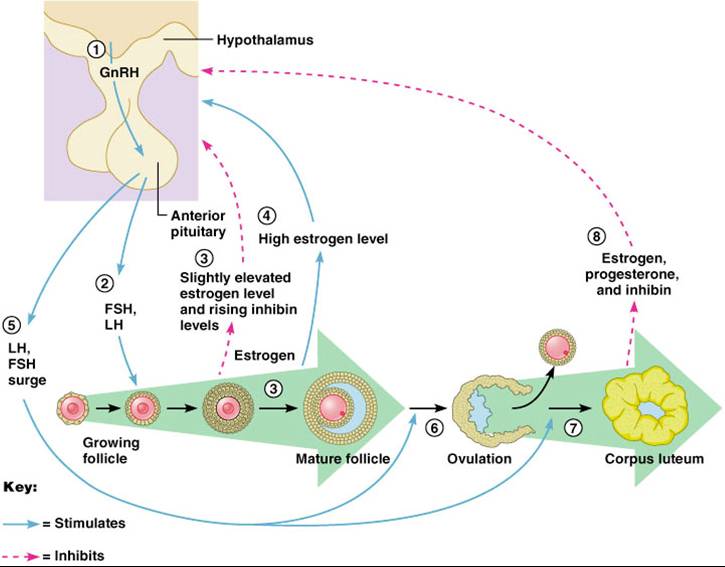
Hormonal Interactions of Ovarian Cycle
Day 1
- GnRH stimulates the release of FSH and LH which stimulate follicle growth and maturation, and low-level estrogen release
- Rising estrogen levels inhibit the release of FSH and LH and prod the pituitary to synthesize and accumulate these gonadotropins
- Estrogen levels increase and high estrogen levels have a positive feedback effect on the pituitary, causing a sudden surge of LH
- The LH spike stimulates the primary oocyte to complete meiosis I, and the secondary oocyte continues on to metaphase II

Day 14
- LH triggers ovulation
- LH transforms the ruptured follicle into a corpus luteum, which produces inhibin, progesterone, and estrogen
- Estrogen then s huts off FSH and LH release and declining LH ends luteal activity
Days 26-28
- Ovarian hormones decrease
- The blockade of FSH and LH ends and the cycle starts anew

Feedback Mechanisms in Ovarian Function
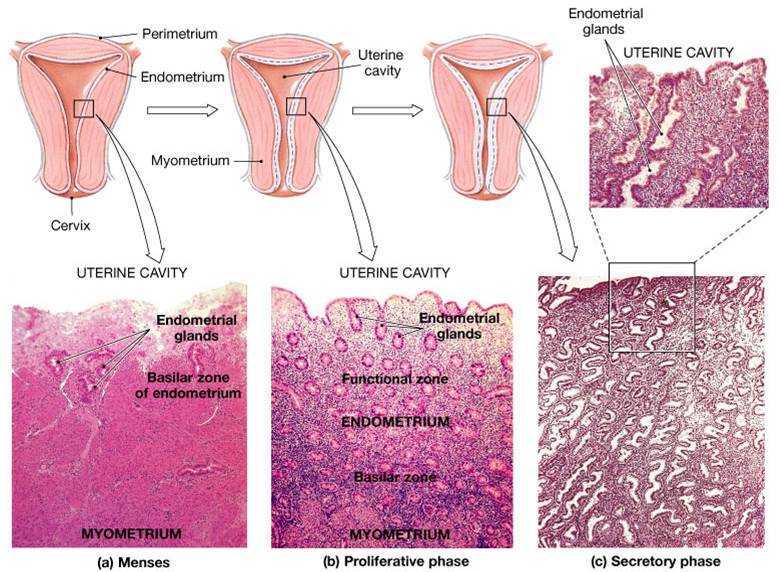
Uterine (Menstrual) Cycle
- Is a series of cyclic changes that the uterine endometrium goes through each month in response to ovarian hormones in the blood
- Days 1-5: Menstrual phase – uterus sheds all but the deepest part of the endometrium
- Days 6-14: Proliferative (preovulatory) phase – endometrium rebuilds itself
- Days 15-28: Secretory (postovulatory) phase – endometrium prepares for implantation of the embryo
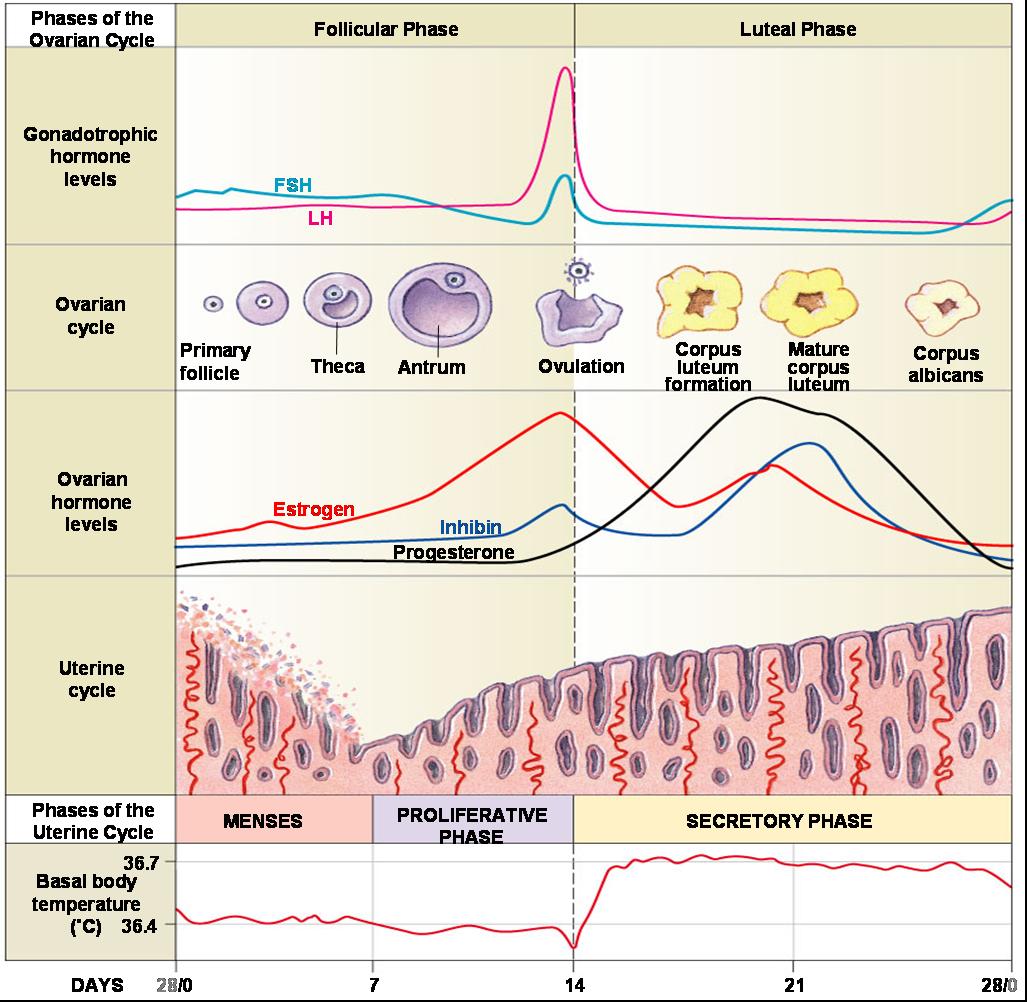
Click here for an animation that will help you understand how hormones are involved in the female reproductive cycle and to understand the ovarian and uterine cycles. |
Menses
- If fertilization does not occur, progesterone levels fall, depriving the endometrium of hormonal support
- Spiral arteries kink and go into spasms and endometrial cells begin to die
- The functional layer begins to digest itself
- Spiral arteries constrict one final time then suddenly relax and open wide, the rush of blood fragments weakens thecapillary beds and the functional layer sloughs
|
 |
Effects of Estrogens and Progesterone
- Estrogen levels rise during puberty
- Promote oogenesis and follicle growth in the ovary
- Exert anabolic effects on the female reproductive tract
-- Uterine tubes, uterus, and vagina grow larger and become functional
-- Uterine tubes and uterus exhibit enhanced motility
-- Vaginal mucosa thickens and external genitalia mature
Estrogen-Induced Secondary Sex Characteristics
- Growth of the breasts
- Increased deposition of subcutaneous fat, especially in the hips and breasts
- Widening and lightening of the pelvis
- Growth of axillary and pubic hair
Female Sexual Response
- The clitoris, vaginal mucosa, and breasts engorge with blood.
- Activity of vestibular glands lubricates the vestibule and facilitates entry of the penis
- Orgasm includes muscle tension, increase in pulse rate and blood pressure, and rhythmical contractions of the uterus
- Unlike males, females do not have a refractory period after orgasm and can experience multiple orgasms in a single sexual experience
Developmental Aspects: Genetic Sex Determination
- Genetic sex is determined by the sex chromosomes each gamete contains
- There are two types of sex chromosomes: X and Y.
- Females have two X chromosomes
- Males have one X and one Y
- All eggs have an X chromosome; half the sperm have an X, and the other half a Y
- A single gene on the Y chromosome, the SRY gene, initiates testes development and determines maleness
Stages of Pregnancy and Development
- Fertilization
- Embryonic development
- Fetal development
- Childbirth
|
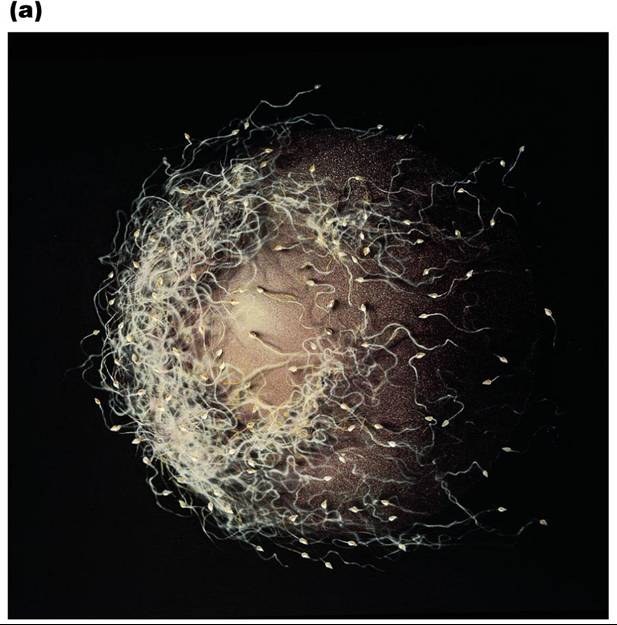
The oocyte is viable for 12 to 24 hours after ovulation. Sperm are viable for 12 to 48 hours after ejaculation.
Sperm cells must make their way to the uterine tube for fertilization to be possible |
 |
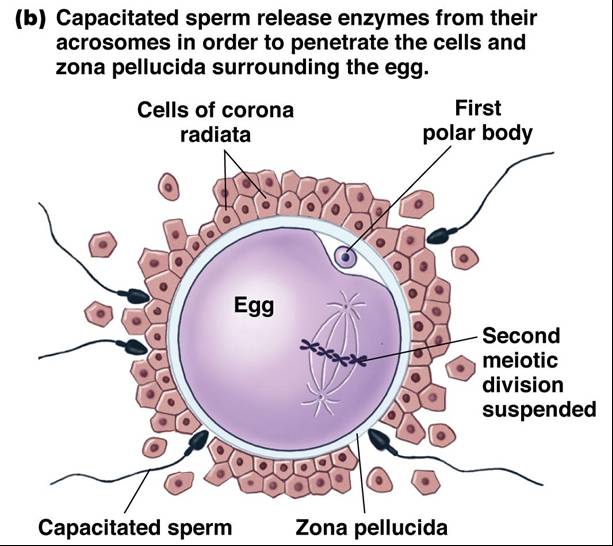
Events Leading to Fertilization
- Sperm binds to the zona pellucida and undergoes the acrosomal reaction
- Fusion of oocyte and sperm plasma membranes takes place
- Membrane receptors on an oocyte pulls in the head of the first sperm cell to make contact
- The membrane of the oocyte does not permit a second sperm head to enter - cortical reaction - enzymes prevent any other sperm from binding to the egg
- The oocyte then undergoes its second meiotic division
- Fertilization occurs when the genetic material of a sperm combines with that of an oocyte to form a zygote
|
 |
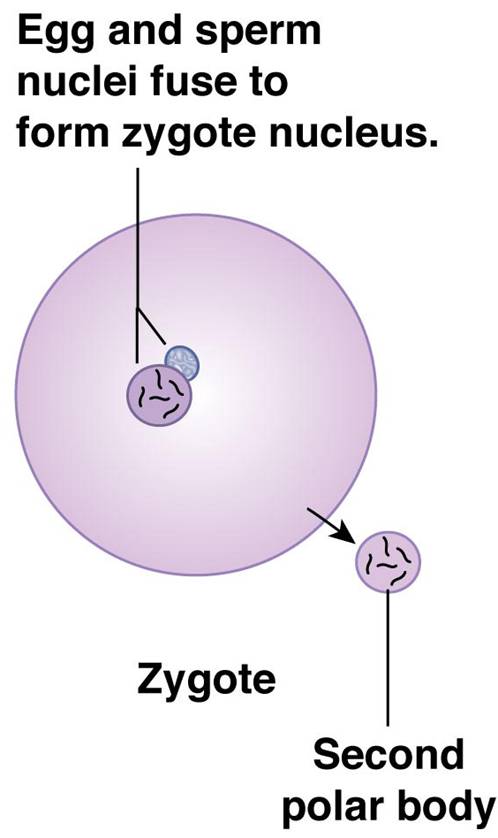 |
Zygote -
- A zygote is the first cell of a new individual, the result of the fusion of DNA from sperm and egg
- The zygote begins rapid mitotic cell divisions
- The zygote stage is in the uterine tube, moving toward developmental stage from the start of cleavage until the ninth week
- The embryo first undergoes division without growth the embryo enters the uterus at the 16-cell state and floats free in the uterus temporarily
- Uterine secretions are used for nourishment
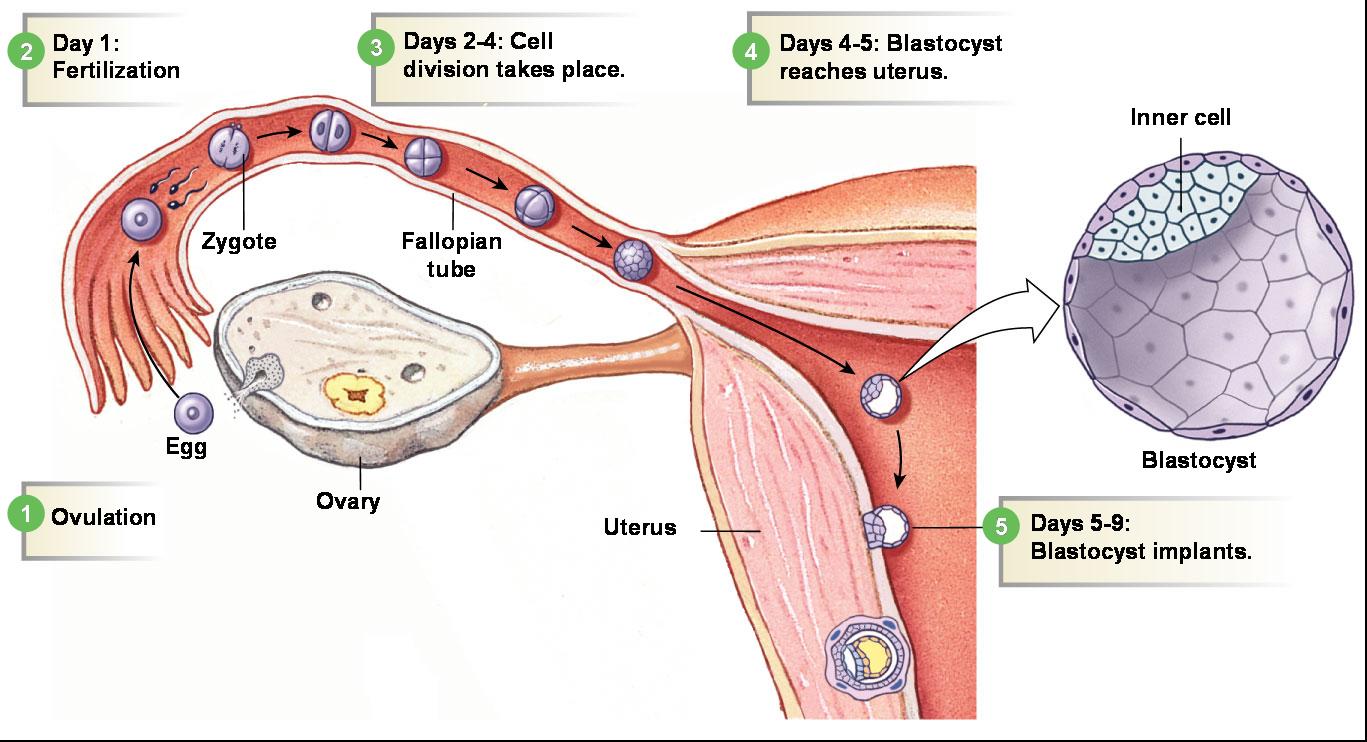
Blastocyst
- A blastocyst is a ball-like circle of cells, begins at about the 100 cell stage
- Consists of an inner cell mass and outer trophoblast
- Secretes human chorionic gonadotropin (hCG) to produce the corpus luteum to continue producing hormones.
- The blastocyst begins implantation in the wall of the uterus about 6 days after conception and completed by day 14
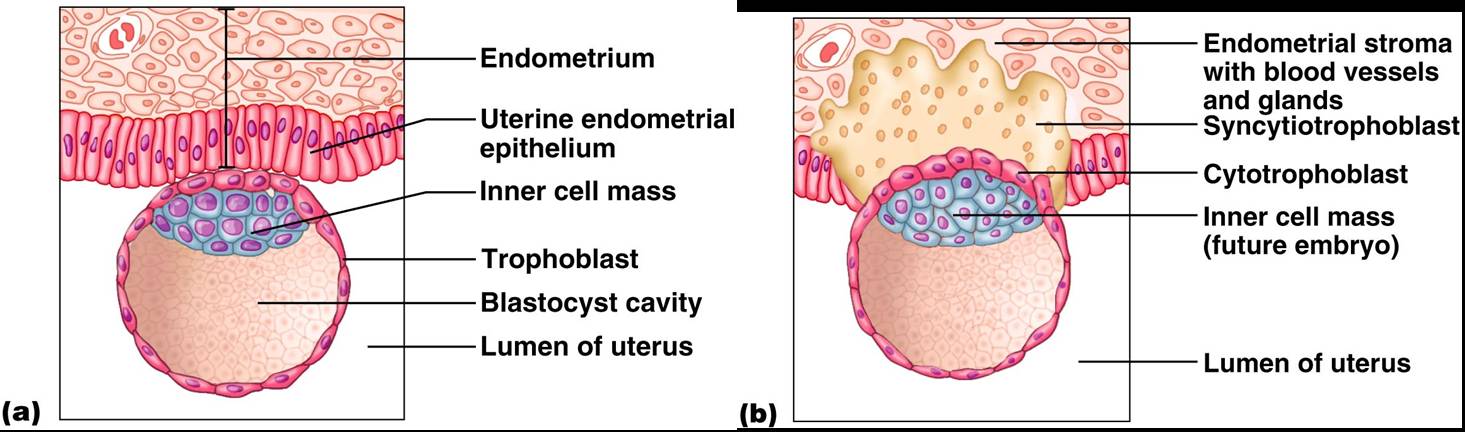
After Implantation
- The chorionic villi (projections of the blastocyst) develop and cooperate with cells of the uterus to form the placenta.
- The embryo is surrounded by the amnion (a fluid filled sac)
- An umbilical cord forms to attach the embryo to the placenta
- The placenta creates a barrier between mother and embryo (blood is not exchanged)
- Delivers nutrients and oxygen
- Removes waste from embryonic blood
- Becomes an endocrine organ and takes over for the corpus luteum by producing
estrogen, progesterone and other hormones that maintain pregnancy
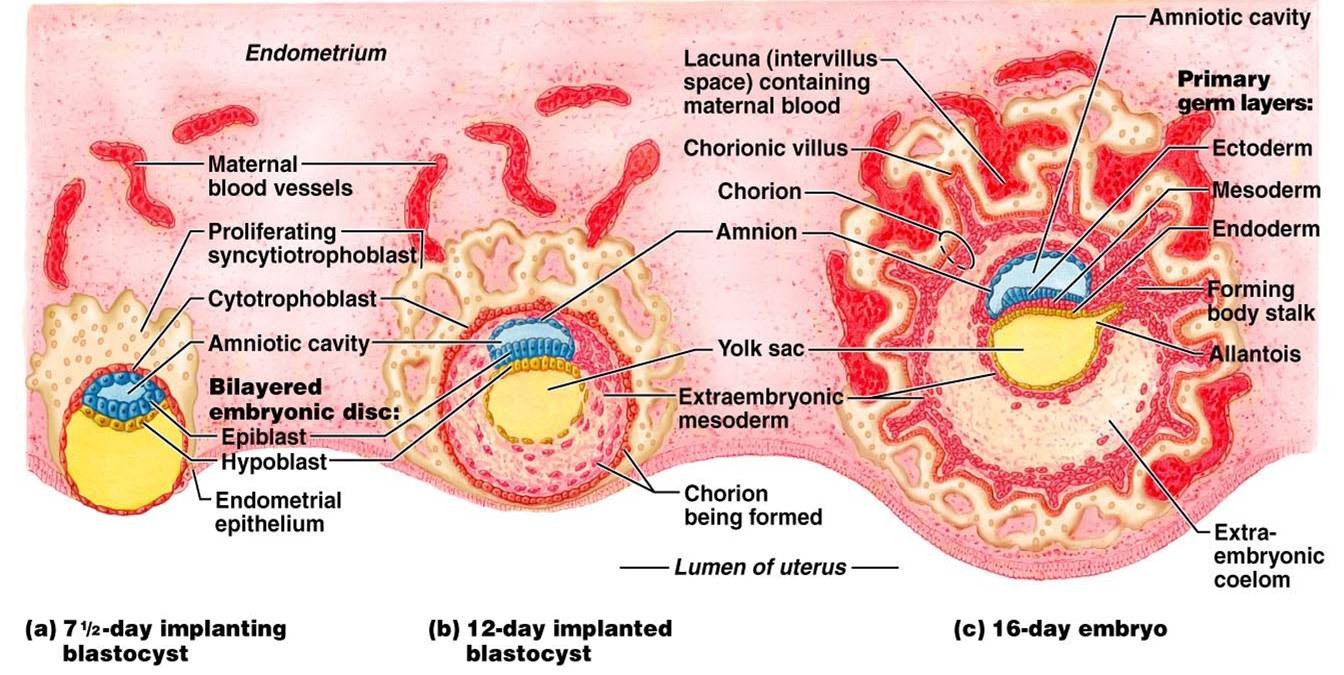
Developmental Aspects
- 5th week – gonadal ridges form and paramesonephric (Müllerian) ducts form in females
- mesonephric (Wolffian) ducts develop in males
- Shortly later, primordial germ cells develop and seed the developing gonads destined to become spermatogonia or oogonia
- Male structures begin development in the 7th week; female in the 8th week
- External genitalia, like gonads, arise from the same structures in both sexes
- All organ systems are formed by the end of the eighth week.
- Activities of the fetus are growth and organ specialization - a stage of tremendous growth and change in appearance

Reproductive Organs at Birth
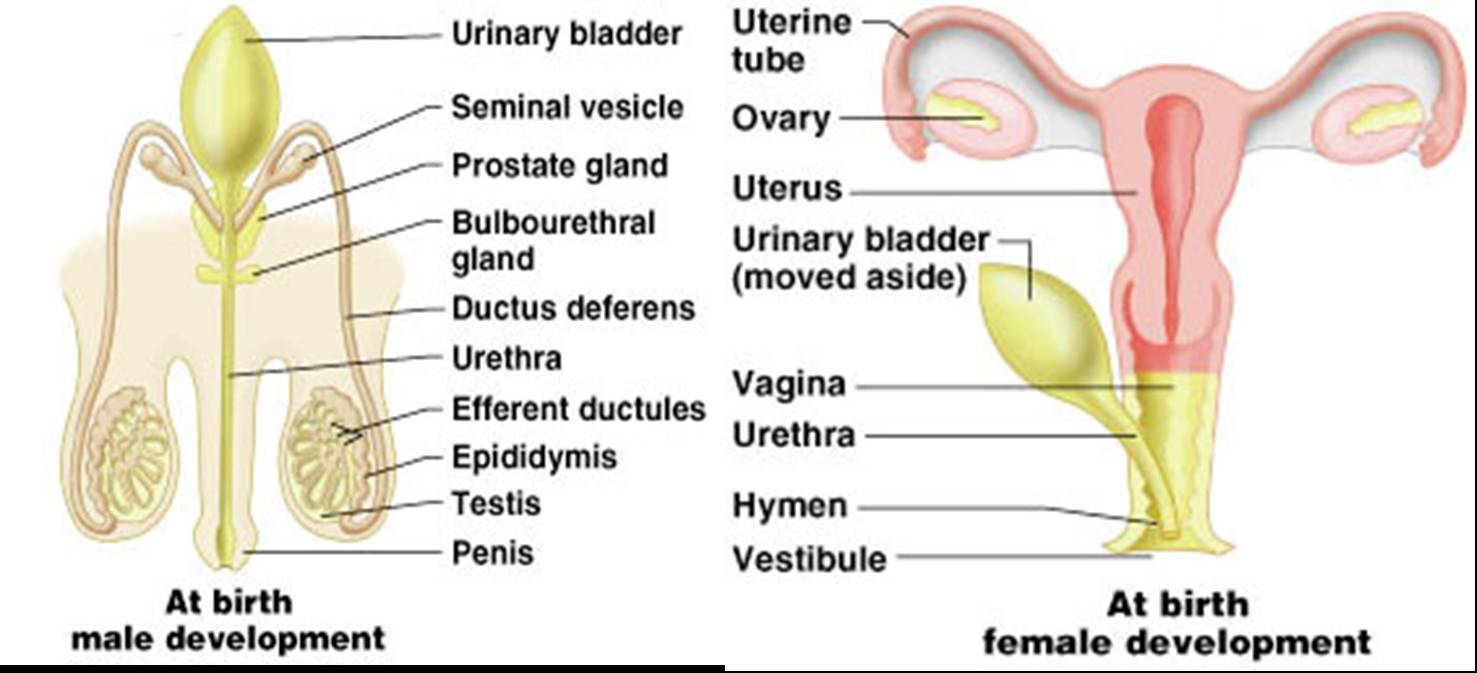
Top ...... Main Page |




 #
#









